A Veterans Administration study that indicates that Iraq and Afghanistan veterans with vision loss from traumatic brain injury have significantly poorer quality of life than comparable civilian patients is part of the scientific program at the joint meeting of the AAO and PAAO today.
The program also includes a Harvard doctor's insights on how to best evaluate and care for low-vision patients who experience vivid visual hallucinations due to Charles Bonnet syndrome.The AAO-PAAO meeting, the largest, most comprehensive ophthalmic education conference in the world, is in session October 24 through 27 at the Moscone Center, San Francisco.
Quality of Life Worse for Veterans with TBI Vision Loss than for Comparable Civilians
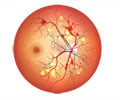
Many young veterans of the Iraq and Afghanistan wars suffer traumatic brain injury (TBI) from exposure to combat explosions. A recent study of TBI's affect on visual function and quality of life in such veterans by Glenn C. Cockerham, MD, Stanford University, and colleagues at the Veterans Administration Palo Alto Department of Ophthalmology, found that most had severe vision problems and poorer quality of life than comparable civilian patients.
Dr. Cockerham, Sonne Lemke, PhD, Catherine Glynn-Milley, CRNO, and Kimberly Cockerham, MD, assessed visual function and occult (not readily detectable) eye injuries in 42 young veterans with blast-related TBI, then evaluated them using two standard quality of life tests, the National Eye Institute Visual Function Questionnaire (VFQ-25) and Neuro-Ophthalmic Supplement (NOS). The veterans' VFQ-25 and NOS scores were compared with accepted norms for patients with similar visual disorders. On the VFQ-25, overall scores were significantly lower for veterans than the reference patient groups; for example, veterans scored lower than norms for patients with glaucoma, multiple sclerosis (MS) and diabetic eye disease. On the NOS the veterans' scores were significantly lower than norms for patients with MS and disease-free adults and were similar to norms for comparable neuro-ophthalmic patients.
The eyes and related tissues are less protected than the head during explosions and are vulnerable to blast forces. A comprehensive eye exam and neuro-ophthalmic evaluation detect occult injuries that may include: structural damage that can lead to glaucoma, retinal and choroidal damage, optic nerve injury, double vision, visual field changes and other disorders.
Advertisement
Who Parked that Double-Decker Bus in My Living Room?
Advertisement
In high-definition detail, CBS patients may see wild animals in their closets, familiar or unfamiliar people sitting on their couches, or incongruous but realistic images, like a double-decker bus. Others see odd shapes or indistinct colored areas. A person may find it hard to distinguish the hallucination from reality, especially when the image seems to fit its context. CBS hallucinations do not arise from psychological or cognitive disorders.
Dr. Jackson noted that once patients understand the hallucinations' cause, they often learn to ignore them; medication can be tried if a person continues to be upset, but most patients are not bothered by the images. CBS patients are counseled to keep active, with the lights bright and music on, since hallucinations are more likely during quiet periods. Visual hallucinations have been induced in normal subjects who were blindfolded for several days for research purposes; Dr. Jackson explained that when the brain's occipital cortex is deprived of visual information, a spontaneous release in the form of hallucinations may occur in the visual association area. Vision and the brain researchers are intensely interested in this phenomenon and its relation to CBS.
Source-Eurekalert
RAS