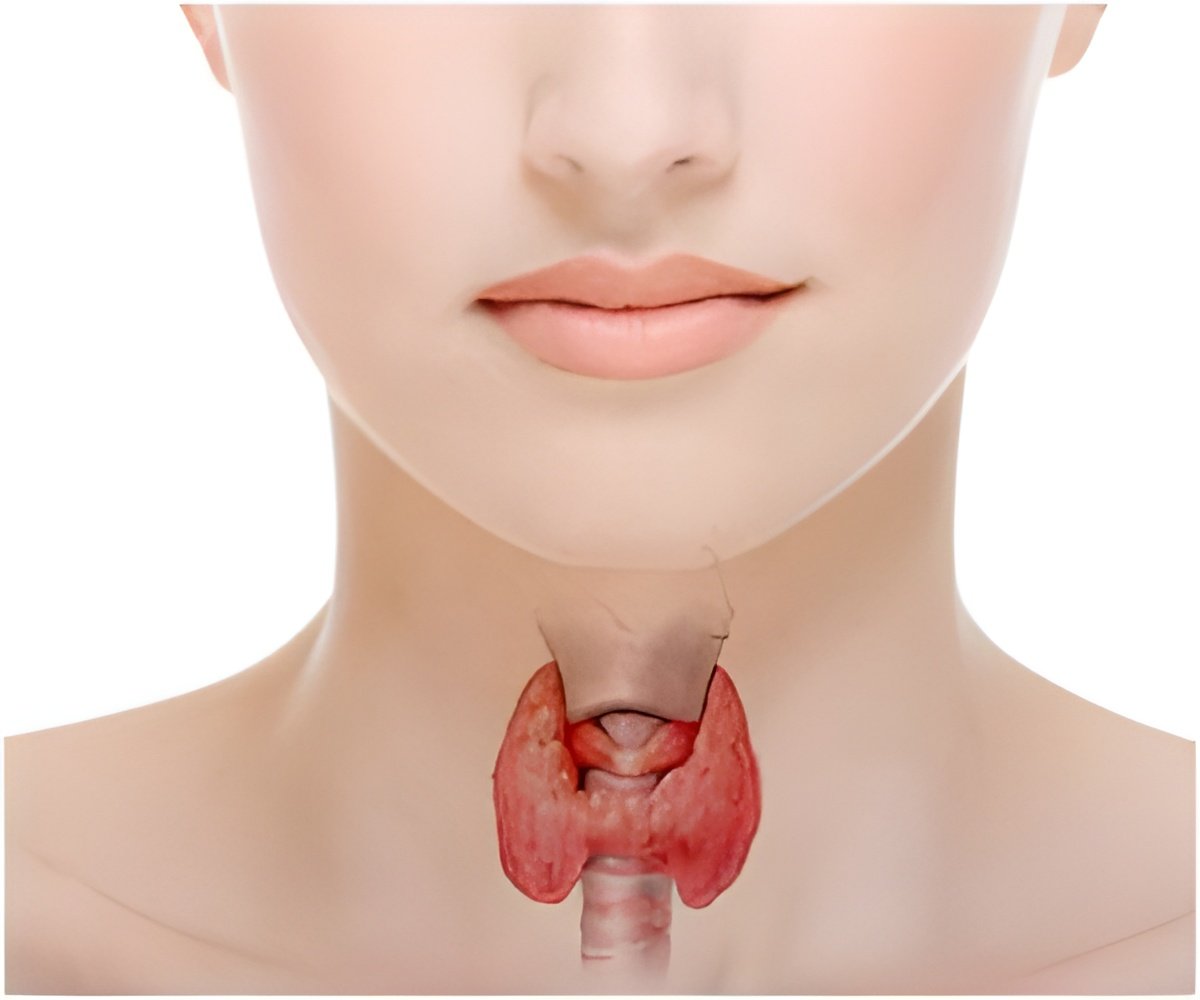
In Graves' disease, the thyroid gland never stops. Thyroid-stimulating antibodies bind to receptors, activating them to keep the thyroid hormone coming and coming and causing the body problems in regulating energy, controlling other hormones and maintaining cells throughout the body.
The findings establish the effect of the receptor antagonist on human thyroid cells.
The antagonist has not yet been tested in animals or people and still has multiple steps of toxicology and safety testing before it may be ready for human trials.
Though treatments are available for hyperthyroidism caused by Graves' disease, including surgery, radioactive iodine, and anti-thyroid drugs, the relapse rates for these treatments are 5 percent, 21 percent and 40 percent, respectively, and each comes with unfavourable side effects.
"Our goal is to develop an easily produced, orally administered, safe and effective drug with few to no side effects that can be used in place of some of the more invasive treatments of hyperthyroidism caused by Graves' disease," said senior author Marvin Gershengorn.
Advertisement
The team is also working on the flip side of thyroid regulation. By researching the thyroid-stimulating hormone receptor, they are hoping to use drug-like compounds to stimulate this receptor to treat people with thyroid cancer, who need more stimulation of thyroid cancer cells to increase the efficacy of iodine radiation.
Advertisement
The findings are published in the Journal of Clinical Endocrinology and Metabolism.
Source-ANI








