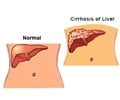
Acetaminophen (Tylenol and generics) is one of the most commonly used over-the-counter drugs in the United States. While generally safe, acetaminophen is known to cause severe liver injury if taken in high doses. But likely due to genetics, even the recommended dose can induce serious liver damage in a significant number of people. In a study published online in Genome Research, scientists have found a genetic marker linked to the risk of acetaminophen-induced liver injury, using a strategy that will help develop safer drugs in the future.
Acetaminophen is considered safe over long-term use, but recent studies have indicated that even over a relatively short period, the maximum allowable dose can induce elevated levels of the liver enzyme ALT in blood serum in approximately one third of healthy individuals, suggesting possible liver injury. It is possible that if given high doses, many of these individuals would be susceptible to acute liver failure. There is likely to be a genetic predisposition, but finding the variants by scanning human subjects alone can be very difficult, requiring large studies with many participants. But with a little help from mice, researchers can overcome these experimental hurdles.In this study, a team of researchers led by Dr. David Threadgill of North Carolina State University utilized mouse genetics to aid the search for candidate genes linked to acetaminophen-induced liver injury in humans. "We approached the study from the perspective that drugs are used in very heterogeneous patient populations, and that drug-induced toxicities are likely the result of a person's genetic makeup," Threadgill explained. The group used a genetically diverse population of mice to model human genetic variation, taking advantage of the known genetic differences in these strains to find genes linked to variable responses to acetaminophen treatment.
Once Threadgill and colleagues narrowed their search to a few candidate genes in mouse, they sequenced the genetic code of the counterparts of the same genes in human patients exhibiting elevated levels of serum ALT in response to acetaminophen. They found that a single letter change to the DNA sequence in one of these candidate genes, called CD44, is significantly associated with elevated serum ALT in these patients. While the role of this gene in liver toxicity is not yet known, CD44 could serve as a potentially useful marker to identify people at risk for acetaminophen-induced liver damage.
Threadgill noted that in addition to the identification of a gene linked to acetaminophen-induced liver injury, this study has broader implications for drug testing, as up until now, genetic differences in humans has not been considered in pre-clinical tests using animal models. "If genetic differences are included in early safety testing, more accurate predictions of clinical response will be obtained," said Threadgill. "The end result will be safer drugs."
Source-Eurekalert
SRM