These cellular changes can also be a precursor to cancer. As in most cancers, early identification of these pre-cancerous cells often leads to better outcomes for patients.
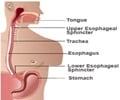
Using an endoscope to reach the esophagus via the nose, physicians shine short bursts of this light at locations of suspected disease and sensors capture and analyze the light as it is reflected back.
UNC gastroenterologist Nicholas Shaheen conducted the preliminary clinical trial of the device on 46 patients with Barrett's esophagus.
The technology that Adam Wax, associate professor of biomedical engineering at Duke's Pratt School of Engineering, and his team developed for cancer detection is known as angle-resolved low coherence interferometry (a/LCI).
The technique is able to separate the unique patterns of the nucleus from the other parts of the cell and provide representations of its changes in shape in real time.
Advertisement
Source-ANI