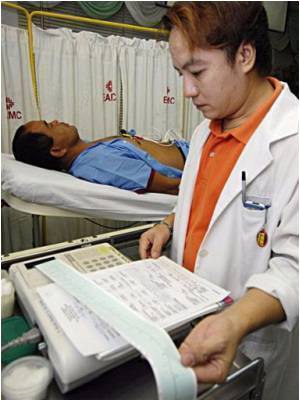
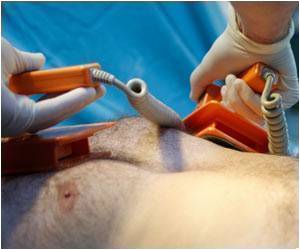
The researchers, led by a team at Ohio State University, believe these neurological problems might relate to inflammation and brain-cell death. The study revealed how the brain is damaged during cardiac arrest, as well as how a drug might counter those effects.
The scientists identified in a mouse model how the loss of blood in the brain sets off a process that attracts inflammatory compounds and kills brain cells. The study showed that these damaging effects were associated with alteration of the cholinergic system - an area of the brain that sends signals using the neurotransmitter acetylcholine to regulate inflammation.
Mice that were treated with an experimental drug called GTS-21, which ctivates acetylcholine, had lower levels of inflammatory chemicals and reduced damage to brain cells in the days following a surgically induced cardiac arrest and subsequent resuscitation.
"This is a drug that has been used safely in humans in clinical trials, so we think our findings have significant clinical potential," said Courtney DeVries, professor of neuroscience and psychology at Ohio State University and senior author of the study. "Another very important aspect of the study is that the drug was not given until 24 hours after resuscitation, and yet it was successful at reversing inflammatory effects in the brain. So there would be a large therapeutic window of time if this could eventually be used clinically."
The research is published in the March 2 issue of The Journal of Neuroscience.
Advertisement