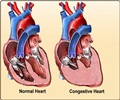
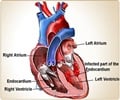
Heart failure is diagnosed when the heart can no longer provide sufficient blood to the body.
"You've had sufficient damage to your heart that it doesn't work very well. You collect fluid in your lungs, you swell up, and you have trouble breathing," Dorn said.
In previous work, Dorn and colleagues used a partial genome-wide search technique to define the region of DNA in which sequence changes were associated with heart failure.
But most of these sequence changes did not code for a change in protein and appeared not to have actually caused the increased risk. Instead, they served as markers, providing clues that this portion of the genome was worth a closer look.
Dorn and his team sequenced the neighbouring gene, looking for variations in parts of the DNA sequence that do code for proteins.
Advertisement
A single change in the DNA sequence of a gene called CLCNKA leads to a change from arginine to glycine in the 83rd amino acid of the protein. This protein makes up part of a kidney channel responsible for controlling the secretion of chloride ions into the urine, an important process in maintaining the proper balance of salt and water in the body.
Advertisement
Renin is produced in the kidney and is the first signal in a cascade that can damage the heart. This opens the possibility of helping people who have the variant reduce their risk of heart failure with drugs commonly used to treat high blood pressure, including ACE-inhibitors and aldosterone blockers.
"There are lots of people walking around with this variant who don't have heart failure," Dorn said.
"But we think if you have this predisposition and something else happens to you, such as developing high blood pressure or having a small heart attack, that increases your odds of developing heart failure."
The study appears Jan. 17 in The Proceedings of the National Academy of Sciences.
Source-ANI