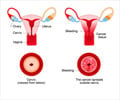
Cystoscopy, the standard for screening for recurrence of early-stage bladder cancer, is a cost-effective method of detecting tumors, a new study from The University of Texas M. D. Anderson Cancer Center, researchers has found.
Adding other tests to cystoscopy increases the cost, as well as the number of false positives that may result in emotional distress and unnecessary procedures, the investigators include.The study was presented today in advance of the American Society of Clinical Oncology (ASCO) Genitourinary Cancer Symposium. Jose Karam, M.D., a fellow in M. D. Anderson''s Department Genitourinary Oncology, presented the findings.
"Our research potentially will enable clinicians to make judicious use of the available ancillary ''urinary markers,'' which would translate into costs savings plus less anxiety for bladder cancer patients," said Ashish Kamat, M.D., associate professor of Urology and director of M. D. Anderson''s Urologic Oncology Fellowship Program.
"The tests frequently added to cystoscopy have many more false positives than commonly believed, and they can lead to unnecessary work-ups. Our findings also may help reduce the cost of caring for bladder cancer patients, which currently in is the range of $4 billion annually," continued Kamat, the study''s senior author.
Early-stage bladder cancer, or non-muscle invasive bladder cancer (NMIBC), has a high rate of recurrence. Patients are tested every three to six months, often for the rest of their lives, with the goal of catching the cancer early if it returns.
Cystoscopy is an outpatient procedure in which a tiny tube with a small camera attached is inserted through the urethra into the bladder. Doctors then are able to visually examine the inside of the bladder for tumors. Many times, in efforts to ensure accuracy and early detection of bladder cancer recurrence, other tests are added to cystoscopy.
Advertisement
Kamat and his colleagues prospectively evaluated 200 M. D. Anderson patients with NMIBC. They compared the accuracy and cost of cystoscopy alone and cystoscopy combined with:
Advertisement
* NMP22, a urine test that tests the level of NMP22 protein
* FISH (fluorescence in situ hybridization), a urine test for chromosomal aberrations in bladder cells
* NMP22 confirmed by FISH
By looking at the number of tumors detected and the cost of the tests (based on Medicare 2009 data) plus the cost of work-up for a false positive result, researchers arrived at a cost per tumor detected for each method. Cystoscopy alone was the least expensive at $7,692, while cystoscopy plus FISH was the priciest at $19,111.
But despite their added costs, additional tests did not give better results. Cystoscopy was most cost effective in finding tumors. Cystoscopy had two false positives, the fewest of any test, while cystoscopy plus FISH had the most false positives at 30.
"There are some who believe that the ancillary tests have the property to predict recurrences early," Kamat said. "In order to account for this, we took into account tumors detected later - at the first follow-up - to assess whether the tests added to detection rates. Our results suggest that, while the ancillary tests did turn positive prior to actual tumor recurrence in a handful of patients, the vast majority were still falsely positive."
Kamat said he would like to see the findings of this study confirmed in the near future by a multi-center co-operative study.
About M. D. Anderson
The University of Texas M. D. Anderson Cancer Center in Houston ranks as one of the world''s most respected centers focused on cancer patient care, research, education and prevention. M. D. Anderson is one of only 39 Comprehensive Cancer Centers designated by the National Cancer Institute. For six of the past eight years, M. D. Anderson has ranked No. 1 in cancer care in "America''s Best Hospitals," a survey published annually in U.S. News and World Report.
Source-Newswise
RAS