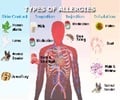
A new study has found that Irritable Bowel Syndrome (IBS) is likely to be higher in patients with allergies.
The study was conducted on 125 adults by Mary C. Tobin, M.D, Department of Immunology/Microbiology at Rush University Medical Centre, Chicago, and colleagues.They found that IBS was higher in patients with seasonal allergic rhinitis by 2.67 times, in patients with allergic eczema by 3.85 times, and in patients with depression by 2.56 times, suggesting a link between atopic disorders and IBS.
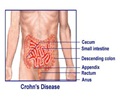
IBS or spastic colon is a functional bowel disorder, affecting about 15 percent of the general population. It appears in a cluster of symptoms including abdominal pain for 12 weeks within the past year, change in bowel habits, stool consistency or frequency, and relief of abdominal pain with defecation.
Various findings suggest indirectly that allergen exposure may lead to IBS symptoms in some patients, but the frequency has not been studied.
“The reported presence of allergic dermatitis was highly correlated to the presence of IBS in our population,” investigators noted.
“In atopic disease, allergic dermatitis is the first step of the ‘atopic march.’ In early childhood, AE (allergic eczema) is frequently associated with gastrointestinal dysfunction and food allergy. A clinical history of AE may be a useful marker for patients with gut hypersensitivity and atopic IBS,” they added.
Advertisement
Authors propose that, “this subgroup of IBS (atopic IBS) be considered separately from patients with IBS without atopic symptoms, because they may have distinct pathophysiologic features and may benefit from specific therapeutic interventions.”
Advertisement
Source-ANI
LIN/K