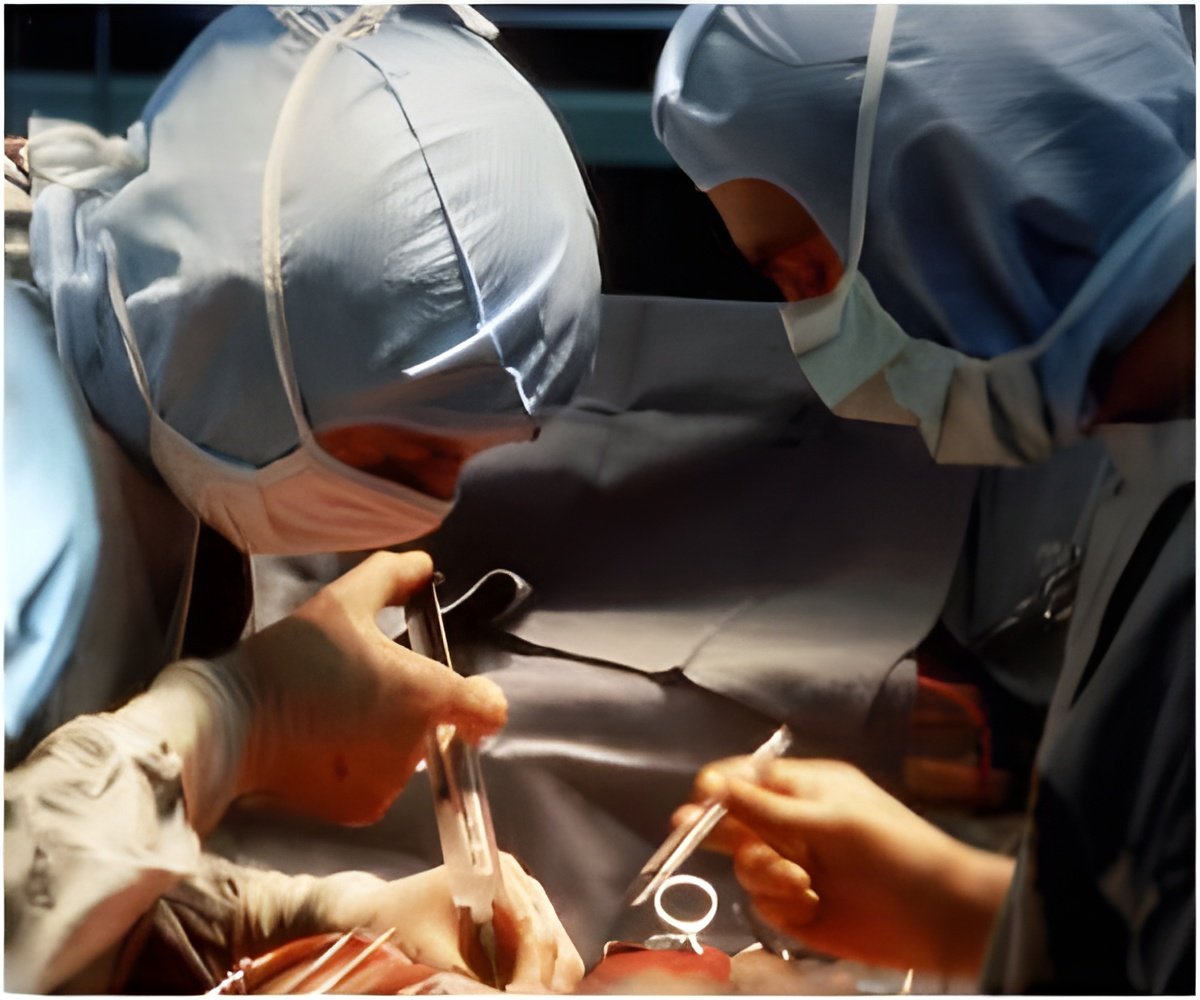
The procedure they looked at is known as EVAR (endovascular aortic aneurysm repair), an operation that surgeons perform to repair a bulging aorta to prevent it from rupturing. EVAR is far less invasive than conventional open-chest surgery, but it requires the surgeon to undergo specialized training. Also, a portable angiography device must be on hand to guide the catheters that place a sheath to repair the aortic bulge. EVAR involves inserting a catheter and a guidewire in the groin and manipulating that to feed the sheath-like device along with a stent graft through the femoral artery and into the aorta, which is located above the heart. A balloon expands the stent to seat the sheath at the bulge in the aorta, in effect creating a new aortic wall inside the weakened area. EVAR has been shown to get patients back to normal activity earlier than open surgery and to have fewer post-procedure complications.
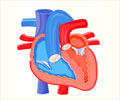
An aortic aneurysm occurs when the wall of the aorta becomes weakened and starts to bulge like a bubble in a tire. Left unattended the aneurysm may rupture, resulting in almost instant death. The aorta is the large arterial structure that transports blood from the heart to the branch arteries throughout the body.
The joint research team from Columbia University Medical Center/New York-Presbyterian Hospital and Mount Sinai School of Medicine mined the Medicare database for 2001 through 2006 to determine how quickly hospitals adapted EVAR in three types of U.S. Census-defined statistical areas: metropolitan with a core city of 50,000 or more; micropolitan with a core city of 10,000 to 49,999; and rural.
"We looked at areas that are truly rural, meaning in terms of population density and they are also isolated from major metropolitan settings in terms of economic or work ties," said lead investigator In-Kyong Kim, MD, Columbia University.
While in the first three years the study found that rural settings lagged far behind the other two in terms of proportion of EVAR for all aortic aneurysm repairs, all three settings evened out by the sixth year, according to Dr. Kim. In 2001, EVAR accounted for almost 30 percent of aortic aneurysm repairs in metropolitan hospitals compared with 5.3 percent in rural settings. By 2006, EVAR accounted for 60.8 percent and 61.3 percent, of aortic aneurysm repairs in metropolitan and rural settings, respectively.
Advertisement
The study is significant because previous research has shown that rural areas do not always have the access to specialized, advanced procedures that urban areas enjoy. A well-documented shortage of surgeons in rural areas has made the problem more acute.
Advertisement
Dr. Kim noted another key event in the early adaptability of EVAR may serve as a model for moving advanced medical procedures into rural and underserved health care settings. She credited the Society for Vascular Surgery with establishing stringent standards and guidelines early in the adaptation of EVAR to minimize complications typical in the early adaptation of a medical procedure.
Natalia Egorova, MPh, PhD and James F. McKinsey, MD, FACS also participated in the study.
Source-Newswise