What is Episiotomy?
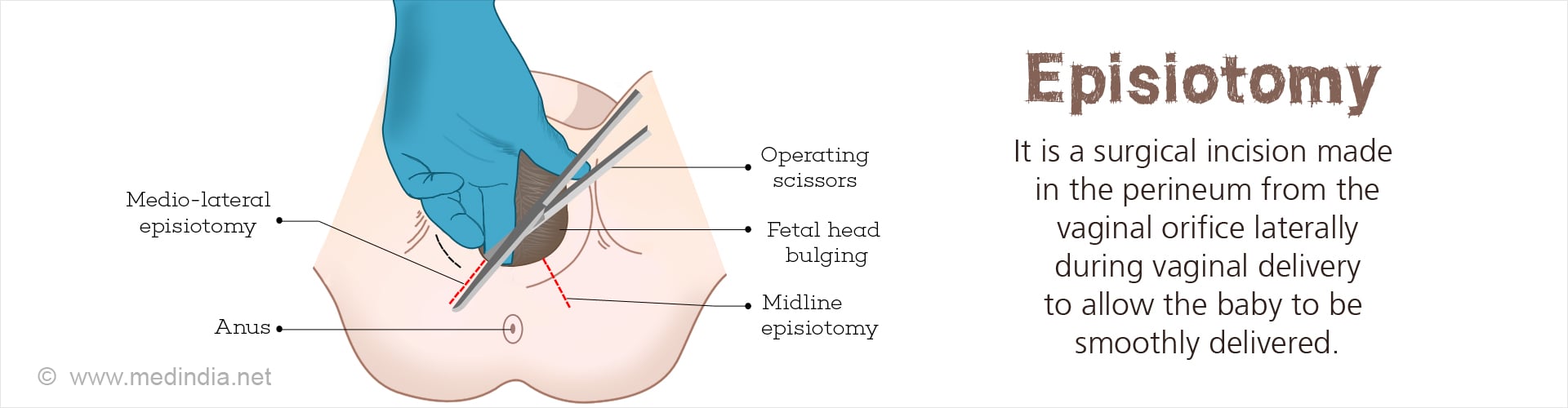
Episiotomy, also known as perineotomy, is a surgical procedure in which an incision is made in the vaginal tissue and the muscle between the vagina and anus, called the perineum. The incision in made just prior to the birth of the baby to enlarge the vaginal opening, thereby facilitating the delivery of the baby.
Historically, it is said that the obstetrician Sir Fielding Ould first described episiotomy way back in 1742, in his Treatise of Midwifery in Three Parts. The procedure became popular in the early 20th century largely due to the efforts of Dr. Joseph DeLee, a well-known obstetrician from Chicago, USA.
Although episiotomy was a routine part of normal childbirth in the early days, with the advancement in knowledge, it is now recommended only for certain cases. Therefore, in recent times, episiotomy rates have decreased appreciably throughout the globe. The episiotomy rate in India is difficult to ascertain, although some studies have shown that it may range between 53-77%, but can be as high as 92% in case of deliveries at private hospitals. Therefore, the evidence-based recommendation of limiting the episiotomy rate to below 30%, is far less than what is actually practiced in India.
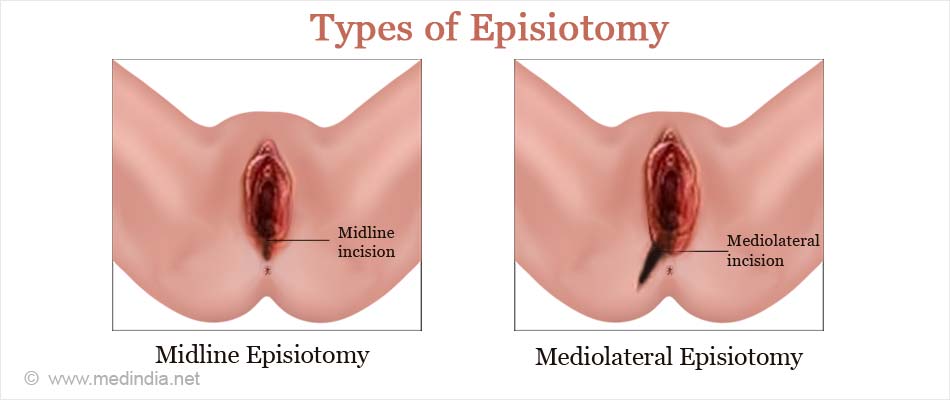
There are two types of episiotomy midline and mediolateral, both with their advantages as well as disadvantages.
- Midline Episiotomy: This type of episiotomy involves an incision from the vagina straight down towards the anus. This type of episiotomy is less painful. The major advantages of this type of episiotomy are (i) reduced blood loss, (ii) improved healing, and (iii) less painful sexual intercourse. The major disadvantage of this procedure is that the tear can extend into the anal muscles that can lead to problems in the long-run, such as fecal incontinence.
- Mediolateral Episiotomy: This type of episiotomy involves an incision that extends from the vagina at a 45° angle to the vaginal orifice. The incision may be made on either the left or right side. The major advantage of this type of episiotomy is that the chances of anal muscle tear are much less. The major disadvantages include (i) greater blood loss (ii) slow healing (iii) more pain, and (iv) difficult and painful sexual intercourse (dyspareunia).
Classification of Episiotomies Based on the Extent of the Tear
Episiotomies are classified on the basis of the extent of the tear into the following four categories:
- First Degree: In this type of episiotomy, the tear only penetrates the vaginal lining.
- Second Degree: This is the most common type of episiotomy, where the tear penetrates the vaginal lining and the underlying vaginal tissues.
- Third Degree: In this type of episiotomy, the tear extends through the vaginal lining, vaginal tissues and part of the anal sphincter.
- Fourth Degree: This is the most severe of the four types of episiotomies. In this type of episiotomy, the tear extends through the vaginal lining, vaginal tissues, anal sphincter and the rectal lining.
It is to be noted that with increasing severity of the episiotomy, the chances of complications like severe pain and infections also increase proportionately. In most cases, obstetricians aim for a second degree episiotomy, which could unintentionally extend to a third or a fourth degree.
It is important to note that episiotomy is not recommended in case of spontaneous vaginal delivery. However, the procedure can be done in the following conditions:
- If the baby is in distress (increased/decreased heart rate) and there is a serious risk to the babys life if not born quickly.
- If the baby is larger than normal (fetal macrosomia).
- If there is a clinical need for forceps delivery or vacuum delivery.
- In case of breech birth, in which the baby is not born head-first.
- If the mother is exhausted from a prolonged labor.
- If the mother suffers from a serious health condition and a speedy delivery is required to keep her safe.
Both types of episiotomies (midline or mediolateral) are relatively straight-forward and easy to perform. Episiotomy is done under local anesthesia. In order to perform the episiotomy, the obstetrician will wait till the babys head protrudes approximately 4 cm through the vaginal opening.
This is termed as baby crowning. Once crowning occurs, the obstetrician will insert two fingers into the vagina to protect the babys head from coming in contact with the surgical scissors. An incision will then be made either straight down towards the anus (midline incision) or at an angle of ~45° to the vaginal orifice (mediolateral incision). The perfect timing for the episiotomy is when the baby is about to be delivered (within the next 3-4 contractions).
This type of accuracy in the timing of the episiotomy is also associated with far lesser blood loss. After the incision is made, the obstetrician will use his/her fingers to pinch the skin below the incision to ensure that further unnecessary tearing does not occur. He/she will also apply gentle pressure on the babys head to prevent it from coming out too abruptly so that the delivery occurs as smoothly as possible.
After the delivery of the baby and the placenta, the vagina and perineum are cleaned and thoroughly examined for any extension of the episiotomy. The anal canal is also checked to exclude anal sphincter injury. The episiotomy is then repaired by suturing the vaginal lining and the underlying tissue. The sutures are dissolvable and are absorbed by the tissues usually within a month. So, there is no need to visit the doctor to take out the stitches.
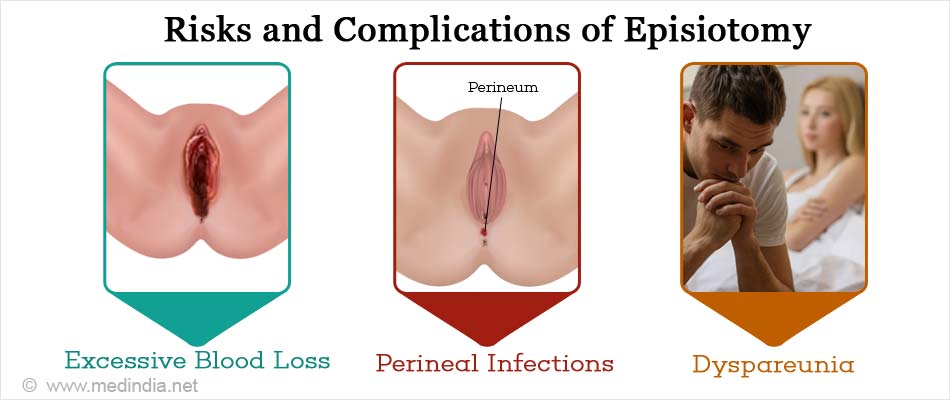
As with any surgical procedure, episiotomy is not without risk. Complications can arise due to penetration of the episiotomy incision into deeper structures, as well as due to various other reasons. The major complications are briefly highlighted below:
- Excessive Blood Loss: This can occur either at the time of the episiotomy or after the repair.
- Extension of the wound: The wound may extend beyond its intended limits. It may also include the anal region resulting in fecal incontinence
- Perineal Infections: Infections are very rare, but can nevertheless occur. Necrotizing fasciitis is a rare but potentially fatal complication of episiotomy. Moreover, methicillin-resistant Staphylococcus aureus infection arising from the episiotomy site has also been reported.
- Postpartum Perineal Pain: Excessive perineal pain after childbirth can be a sign of the formation of a hematoma, a blood clot in the wound.
- Wound Dehiscence: Wound dehiscence is the rupture of the stitched-up wound along the line of incision that can occur after an episiotomy. However, dehiscence of an episiotomy usually occurs less than 2% of the time.
- Dyspareunia: This is commonly known as painful sexual intercourse. It can last anywhere up to 18 months postpartum. Episiotomy during first birth and scarring of the perineum during the procedure are major risk-factors for long-term dyspareunia.
![Risks and Complications of Episiotomy Risks and Complications of Episiotomy]()
The recovery period varies with the type of episiotomy performed. In case of first or second degree episiotomy, the recovery will be faster than in case of third or fourth degree episiotomy. In the latter cases, the pain will last longer. On an average, it can take about a month for the episiotomy wound to heal and the stitches to be dissolved. During this period, follow the doctors advice to facilitate the healing process. Some simple strategies are given below:
- Ease the pain: Painkillers can be taken as advised by your doctor to ease the pain. Acetaminophen or paracetamol is the safest choice, since it can be taken even while breastfeeding. You can take ibuprofen if your baby is not premature or of low birth weight and does not suffer from any other health issues. Diclofenac gel patches applied to the perineum can also ease the pain. Since ibuprofen and diclofenac are both non-steroidal anti-inflammatory drugs (NSAIDs), they not only take care of the pain, but also reduce inflammation and swelling. Aspirin is not recommended as it can pass to your baby through the breast milk.
- Soothe the wound: Cool the wound by placing an ice-pack or ice-cubes wrapped in cloth on the affected area. This will have a soothing effect and also help to ease the pain.
- Keep the wound clean: Keep the episiotomy wound and the surrounding area clean. Rinse the perineal region with warm water after defecation and urination.
- Avoid pressure on your stitches: Your doctor may prescribe a laxative to ease constipation. This will reduce the pressure on your stitches during bowel movements.
- Do pelvic floor exercises: Resume your pelvic floor exercises as soon as possible after birth. These exercises will strengthen the muscles of the pelvic floor as well as increase the blood circulation, thereby aiding the healing process.
As healing occurs, the pain and discomfort will gradually disappear. If however, you experience intense pain at the wound site or develop a fever or if pus oozes out of the wound, you should consult your doctor immediately, as these could be signs of infection.
Health Tips
- Massage your perineum during pregnancy: Starting around 34 weeks of pregnancy, massage your perineum gently using a vegetable-based massage oil. The technique involves placing your fingers around 5 cm (2 inches) inside your vagina and pressing downwards towards the anus. Then move to each side in a U-shaped stretching movement. Daily perineal massage will increase the area's ability to stretch, leading to less need for an episiotomy and fewer natural tears.
- Be cautious about sex after an episiotomy: You should exercise caution about resuming your sex life after an episiotomy. Give the wound adequate time to heal and the pain to fully subside. Take your doctors advice on when it would be safe to resume sex.
- Be careful about infections after an episiotomy: Be aware of the early signs of infection following an episiotomy. Be careful of the following signs: (i) intense pain, swelling and redness at the wound site; (ii) pus or liquid oozing from the wound; (iii) unusual or putrid smell from the wound; and (iv) fever or chills. If you experience any of these signs you should consult your doctor immediately.
- Seek you doctors advice about medications for relieving constipation: If you suffer from constipation, there is a greater chance of rupturing your stitches due to the pressure during bowel movements. Ask your doctor for suitable medications that can alleviate constipation.