- About Porphyria - (http://ghr.nlm.nih.gov/condition/porphyria)
- Porphyria - (http://www.niddk.nih.gov/health-information/health-topics/liver-disease/porphyria/pages/facts.aspx)
- Besur, S.; Hou, W.; Schmeltzer, P.; Bonkovsky, H.L. Clinically Important Features of Porphyrin and Heme Metabolism and the Porphyrias. Metabolites 2014, 4, 977-1006.
- Roca B, Roca M (2012) Acute Intermittent Porphyria: A Reversible Cause of Cachexia. J Clin Case Rep 2:184. doi: 10.4172/2165-7920.1000184
- Harrison's Principles of Internal Medicine 19th edition
What is Porphyria?
Porphyria is a group of genetic disorders that result in built-up of chemicals called porphyrins in the body.
Porphyrins are normally converted into heme, a constituent of hemoglobin with the help of eight different enzymes. Patients with porphyria lack one of the enzymes necessary to bring about this conversion. Porphyria affects nerves or skin, or both. Skin symptoms tend to get worse in the presence of sunlight. Therefore, patients may prefer to move around after dark. This is the reason why some people refer to porphyria as ‘Vampire disease’.

Porphyria may be classified depending on the site in the body where porphyrins are excessively produced. They are:
Hepatic porphyria: Hepatic refers to the liver. Characteristics of hepatic porphyria include the following:
- Symptoms usually appear in adulthood
- Symptoms are nerve-related and include abdominal pain, and motor and mental symptoms
- Attacks are precipitated by dieting, certain medications and hormonal changes
- Patients are at a higher risk for liver cancer
Erythropoietic porphyria : Erythropoietic refers to the blood. Characteristics of erythropoietic porphyria include the following:
- Symptoms usually appear at birth or early childhood
- Symptoms are skin related and the patient is sensitive to sunlight
- If the fetus is affected, it may be born with a condition called hydrops fetalis
Porphyria can also be classified as:
- Acute porphyria, which mainly affects the nervous system. Some forms of acute porphyria can affect the skin as well. Types of acute porphyria include:
- ALA dehydratase-deficient porphyria
- Acute intermittent porphyria, which is the most common form of acute porphyria
- Hereditary coproporphyria
- Variegate porphyria
The last two forms show skin symptoms as well
- Cutaneous porphyria, which affects the skin and worsens on exposure to sunlight. Types of cutaneous porphyria include:
- Congenital erythropoietic porphyria/Gunther disease
- Erythropoietic porphyria
- Porphyria cutanea tarda, which is the most common form of porphyria
What are the Causes of Porphyria?
Porphyria is a genetic condition resulting from lack of an enzyme required for the production of heme. The deficiency of these enzymes results from mutations in one or more of these genes: ALAD, ALAS2, CPOX, FECH, HMBS, PPOX, UROD, or UROS.
The mode of inheritance varies in different types of porphyria. Some are autosomal dominant, where only one abnormal gene is enough for the disease. Some are autosomal recessive, where the defective genes should be present on both chromosome pairs to manifest the disease. In some cases, the defective genes are present on the X-chromosome.

Environmental factors also play a significant role in the development of porphyria. Smoking, alcohol, stress, hormones, certain medications, chronic illnesses and excessive dieting may trigger porphyria. These conditions stimulate the synthesis of porphyrins, thus causing an attack.
Many cases of porphyria cutanea tarda are not inherited, but occur sporadically. Beside the above factors, high iron content in the body, as seen in conditions like hemochromatosis, can trigger the condition.
What are the Symptoms of Porphyria?
Depending on the symptoms, porphyria can be classified as acute or cutaneous.
Acute Porphyria: Acute porphyria predominantly affects the nervous system and, in some cases, skin symptoms may also occur. It occurs as attacks, which are rarely seen after menopause and before puberty in women. The major symptoms and signs of acute porphyria attack include:
- Severe abdominal pain, with no obvious reason. The patient may also suffer from vomiting, constipation or diarrhea, and urinary retention. Vomiting can cause dehydration and electrolyte abnormalities
- Back and limb pain, tingling, numbness, muscle weakness or paralysis. Paralysis of the respiratory muscles can be life-threatening
- Seizures or psychiatric symptoms like anxiety or restlessness, confusion, hallucinations
- Increase in heart rate and high blood pressure
- Red urine, which may change color on exposure to light or air
Cutaneous Porphyria: This form of disease principally causes skin symptoms, especially photosensitivity reactions, where symptoms worsen on exposure to sunlight. It does not affect the nervous system. Certain inherited forms of cutaneous porphyria will begin to show symptoms from infancy or childhood. Cutaneous porphyria may result in the following symptoms:
- Itching and redness of the skin
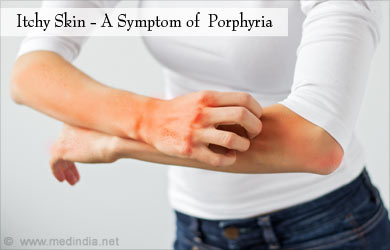
- Skin swelling (edema)
- Blisters on the skin
- Thinning, scaring and color changes of the skin
- Increased hair growth
How is Porphyria Diagnosed?
Porphyria is diagnosed based on the history, physical examination and laboratory tests of the patient. A family history may indicate that other people in the family also suffer from the condition, and therefore gives a clue on the genetic nature of the condition.
Since porphyria is rare, general hospital laboratories do not normally have the expertise, technology or staff to perform porphyria testing. In most cases, testing involves sending samples to a referral laboratory.
Porphyria is diagnosed by analysis of blood, urine, and stool. Urinary porphobilinogen (PBG) is markedly elevated in acute porphyria except for the very rare sub-type due to ALA dehydratase deficiency. Electrolyte abnormalities like low blood sodium levels may be noted on a blood test.
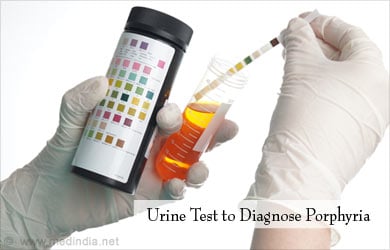
Enzyme testing helps to detect the deficient enzyme and diagnose the exact type of porphyria. Genetic testing can be used to locate the defective gene.
How do you Treat Porphyria?
Treatment of acute porphyria is aimed at reducing or eliminating symptoms and may require hospitalization. The treatment includes the following:
- Stop or reduce the dosage of medications that may have triggered porphyria symptoms
- Intravenous injection of fluids and glucose are administered to maintain an adequate amount of carbohydrates and prevent dehydration. Glucose reduces porphyrin production and is used as temporary treatment till heme can be made available. Oral glucose may be given in the absence of vomiting. The low sodium levels should be corrected
- Hemin injections are given to lower porphyrin levels
- Pain may require narcotic painkillers. Nausea and vomiting, seizures and other symptoms should also be treated
- Liver transplantation may be required in some cases.
Treatment for porphyria cutanea tarda involves the following:
- Treatment with malaria drugs such as hydroxychloroquine or chloroquine. These drugs displace porphyrins from the liver and bring about their excretion in the urine.
- Phlebotomy, the technique used to draw blood from the veins to reduce iron content in the body, This helps to relieve symptoms of porphyria cutanea tarda, which is worsened by excess iron content.
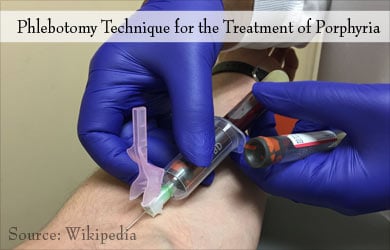
Patients with congenital erythropoietic porphyria and hepatoerythropoietic porphyria are treated with blood transfusions and splenectomy for their anemia.
How do you Prevent Porphyria?
As for other genetic disorders, cases of porphyria can be prevented through genetic counseling. In families affected in porphyria, the defective gene can be located. Depending on its mode of inheritance, couples can be advised the possible chances of transmitting the gene to the children.
Health Tips
Patients with porphyria should take the following precautions:
- Be aware of drugs that can cause porphyria. Do not take any medication without consulting your doctor
- Avoid exposure to sunlight; use sunscreens containing zinc or titanium oxide
- Discuss with your doctor how to identify and prevent symptoms
- Protective clothes should be used to minimize exposed area
- Diets which limit carbohydrate intake should be avoided






