- Hyperhidrosis - (http://www.nlm.nih.gov/medlineplus/ency/article/007259.htm)
- Eisenach JH et al. Hyperhidrosis: Evolving therapies for a well-established phenomenon. Mayo Clin Proc. 2005; 80(5):657-666.
- Schlereth T et al. Hyperhidrosis - Causes and treatment of enhanced sweating. Dtsch Arztebl Int. 2009; 106(3):32-37.
- About Hyperhidrosis - (http://en.wikipedia.org/wiki/hyperhidrosis)
- Natural Remedies - (http://www.sweathelp.org/en/hyperhidrosis-treatments/alternate-therapies.html)
- Stashak AB, Brewer JD. Management of hyperhidrosis. Clin Cosmet Investig Dermatol. 2014; 7:285-299.
- Lee KY, Levell NJ. Turning the tide: a history and review of hyperhidrosis treatment. JRSM Open 2014;5(1):2042533313505511.
- Kennard J, Lopez B. Primary hyperhidrosis: a systematic review. International Journal of Therapy and Rehabilitation 2004; 11(12): 554-549.
What is Excessive Sweating?
There’s a saying that goes like this: Women glow, men perspire and pigs sweat. But anything in excess can make your life miserable. Excessive sweating (hyperhidrosis), especially of the palms, armpits and soles, is a common problem. Besides disrupting normal daily activities, excessive sweating can cause social anxiety or embarrassment. The term hyperhidrosis is derived from the Greek word ‘hidroa’, which means sweat.
Types of Excessive Sweating
The sudomotor system controls perspiration. When the sudomotor system increases the output of sweat, for no obvious reason, it gives rise to the condition of hyperhidrosis or primary hyperhidrosis. Secondary hyperhidrosis occurs in connection with endocrine or neurological disturbances, drugs, injury to the spinal cord, malignancy, or infection. Organophosphate compounds that are used in terrorism warfare or pesticides also contribute to this condition.
Primary hyperhidrosis is classified as generalized or focal. Generalized hyperhidrosis affects several different sites of the body. On the other hand, focal hyperhidrosis affects a particular part. Depending on the part involved, focal hyperhidrosis can be classified as:
- Palmar – Plantar hyperhidrosis, which mainly affects the soles of the feet and the palms of the hands.
- Axillary hyperhidrosis, which is observed in the underarms and may be present along with palmar-plantar hyperhidrosis.
- Craniofacial hyperhidrosis, where the face may also show excess sweating due to emotions, heat, spices (gustatory hyperhidrosis), among others.
Causes of Excessive Sweating
Hyperhidrosis can be caused by many factors and is often observed in children and adolescents. Nearly 3% of the population in the United States is affected with hyperhidrosis, while the same percentage of the population in Southeast Asia is affected with palmar hyperhidrosis. While the exact cause for hyperhidrosis is not certain, there are several factors that are known to initiate the condition.
Family history – Genetics plays a role in excess sweating or primary hyperhidrosis. When an individual suffers from primary hyperhidrosis, there is a high chance of a family member having a similar condition.
Some of the causes of secondary excessive sweating are listed below:
- Medical conditions – Excessive sweating can be a result of tumors, gout, an injury, chronic infections, a hemorrhage, a spinal injury, diabetes or other endocrine abnormalities.
- Intoxicants or medicines – Antidepressants, alcohol, nicotine and organophosphorus compounds can cause generalized hyperhidrosis
- Menopause – Women experience hot flashes during menopause. Certain women experience excess sweating during menopause. This type of sweating is considered secondary hyperhidrosis.

Some of the causes of generalized excessive sweating are as follows:
- Systemic medical conditions – Diabetes, Parkinson’s disease, anxiety, menopause, heart failure, nocturnal sweating, fibromyalgia, drug use, among others
- Brain lesions – Sweating occurs in individuals with episodic brain lesions either with or without hypothermia (drop in temperature).
- Damage to the peripheral nerves (peripheral neuropathy) – Cold exposure sweating syndrome, familial dysautonomia, or a congenital dysfunction of the autonomic nervous system.
- Intrathoracic tumors or lesions
- Spinal cord injuries – Posttraumatic syringomyelia, autonomic dysreflexia
Some of the causes of focal excessive sweating are categorized as below:
- Causes of gustatory sweating – Herpes zoster infections, thoracic sympathectomy, diabetes, encephalitis, syringomyelia, among others
- Associated conditions with hyperhidrosis – idiopathic unilateral circumscribed hyperhidrosis, POEMS syndrome, burning feet syndrome, causalgia, trench foot, glomus tumor, among others
In addition, hyperhidrosis may be associated with thermoregulation, emotions, food, and smells.
Symptoms of Excessive Sweating
The one major symptom of hyperhidrosis is the feeling of being wet in the underarms, face, palms, or soles.
Diagnosis of Excessive Sweating
Doctors initially obtain the medical history of patients with hyperhidrosis. This enables the physician to ascertain the site of hyperhidrosis and the duration of this condition in the individual. Hyperhidrosis can be diagnosed with clinical tests in the following ways:
Dynamic Sudorometry – The quantity of sweat can be measured by quantitative dynamic sudorometry. A ventilated Plexiglas capsule with continuous streaming of air assists in quantitating the sweat released naturally or following stimulation. The effects of therapy to reduce sweating can be determined with dynamic sudorometry.
Thermoregulatory Sweat Test (TST) – In this test, individuals have their bodies coated with alizarin red, sodium carbonate, and cornstarch. Individuals are then placed in a heated chamber called the Guttmann chamber. When the temperature is raised to 38ºC, all individuals start to perspire. However, people with hyperhidrosis tend to sweat excessively even under resting conditions.
Gravimetric Analysis – A piece of filter paper is weighed on a scale with minute precision. The paper is then placed on the area of sweat and weighed again. Sweat production is weighed as mg/min/cm2. This test is used to measure axillary hyperhidrosis.

Minor’s Starch-iodine Test – The test consists of an iodine solution (3.5% iodine in alcohol) that is applied to the sweat producing area with starch added on top of the iodine. The combination of starch and iodine with the sweat results in a violet colour. In the absence of sweat, one does not observe the violet colour. The test helps in determining the location of hyperhidrosis.
Axillary hyperhidrosis is diagnosed when > 50 mg/min of sweat is produced. When the quantity of sweat is > 20 mg/min, palmar hyperhidrosis is diagnosed.
Other tests that help to diagnose any suspected secondary cause of hyperhidrosis should also be carried out.
Treatment for Excessive Sweating
Hyperhidrosis can be treated either surgically, with medications, or with localized treatments. The different forms of treatment are elaborated below:
Surgical Treatment
- Curettage or Liposuction – This procedure is preferred to the previously used surgical excision of the sweat glands. The sweat glands in the underarm can be removed by curettage or by liposuction. The advantage of liposuction is the ease with which the glands are removed with minimal scarring. In terms of aesthetics, complete removal of the glands, and reduced complications, liposuction is a good option for surgical treatment.
- Endoscopic Thoracic Sympathectomy – This procedure was introduced in 1951 and is widely used in the treatment of palmar-plantar hyperhidrosis. This is a minimally invasive procedure. However, there is a complication of excess sweating occurring in a different area from the original site of sweating; this is known as compensatory hyperhidrosis or CH. A recent variation of this procedure is the endoscopic thoracic sympathotomy that reduces the extent of CH.
Localized Treatment
- Antiperspirants – Metal salts, such as aluminium chloride (15% to 25%), or a combination of aluminium chloride hexahydrate and anhydrous ethyl alcohol, present in antiperspirants cause the formation of vacuoles or atrophy in the secretory gland cells, or block the sweat ducts. The area of application should be covered and left for 6 to 8 hours, preferably at night. However, the effect of antiperspirants is temporary and is found to be ineffective in very severe cases of hyperhidrosis. In general, axillary hyperhidrosis is treated with antiperspirants.
- Botulinum toxin type A (BT-A) – It is injected intradermally in the areas of sweating. To tackle the pain involved in the procedure, intravenous anesthesia (regional or sedation), pain-relief ointments, or medications are prescribed. The reduction in sweat is observed within 2 to 4 days and there is a considerable reduction in sweat within a couple of weeks. The therapeutic effect lasts for 7 months before the sweat glands resume their function. This form of treatment is repeated every 4 to 17 months. A dose of 50 to 100 IU is injected into the armpit. The low dosage of the toxin prevents major disruption of the nerves and the overall anti-perspiration effect is considerable. The disadvantage of a BT-A injection into the palms is the pain associated and the possible weakness of the fingers of the palm due to the paralytic effect of the toxin.

- Glycopyrrolate and Clonidine – Craniofacial hyperhidrosis is improved with a daily topical treatment of a 0.5% glycopyrrolate solution. Incremental increase in the dosage of clonidine till it reaches a concentration of 0.3 to 0.4 mg/d has been found to completely inhibit excessive sweating. Clonidine is a sympathetic nerve function inhibitor.
- Iontophoresis – This involves the application of a current from a battery-powered unit through tap water-soaked wool pads on the site of excess sweating. The pads are separated from the site by a nonconducting barrier. Individuals use this apparatus 2 times a day for 30 minutes. There is a significant reduction in sweating in 2 weeks, and the condition is controlled for several weeks before the treatment is resumed. Some of the disadvantages include minor burns due to the current.
Systemic Medications
Anticholinergic drugs, antihypertensive drugs, calcium channel blockers, and antidepressants may be used to treat generalized hyperhidrosis. They display mild to moderate therapeutic effects. Some of the disadvantages to these medications include memory loss, urine retention, dry mouth, constipation, among others.
Alternative Therapies
Chamomile, sage, St. John’s wort, valerian root, relaxation, acupuncture, and meditation are some alternative forms of treatment. However, the efficacy and use of these treatments have not been confirmed. Use of alternative treatment depends on the individual’s decision. One must consult with the physician before resorting to alternative treatments.
Emerging Treatments
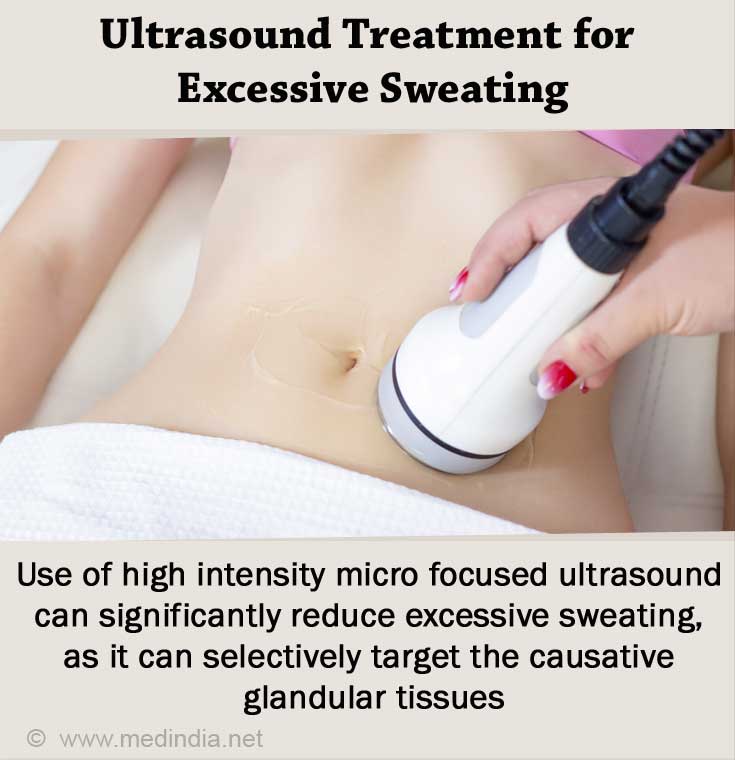
Ultrasound Treatment – Recent research has shown that the use of high intensity microfocused ultrasound can significantly reduce hyperhidrosis, as it can selectively target the causative glandular tissues.
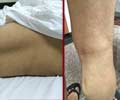
Laser Treatment – This is another minimally invasive technique that can target glandular tissue to reduce sweating. While most individuals show a significant improvement in the reduction of hyperhidrosis, there are some individuals who may show an increased level of sweating in the armpit regions. More research studies need to be performed to confirm the therapeutic role of lasers.
Microwave Treatment – Miramar labs has recently designed a microwave-based device to treat axillary hyperhidrosis. The FDA has approved this device. The microwaves can selectively target the glandular tissues and the dermis layer of the skin. There is a reduction in hyperhidrosis with this treatment. However, there are side effects with this treatment and they include swelling, redness, and weakness in the treated arm. Most of these reactions last a few months to a year.
Different Forms of BT-A Injection – Most individuals experience pain during the administration of BT-A. In recent studies, reconstitution of BT-A with lidocaine helps to prevent or alleviate this pain. This combination reduces the painful effect of BT-A administration. It has also been noted that a combination of iontophoresis with BT-A may be able to alleviate this pain.