- Information About Actinomycosis - (http://patient.info/doctor/actinomycosis-pro)
- About Actinomycosis - (http://www.nhs.uk/conditions/actinomycosis/pages/introduction.aspx)
- What is actinomycosis? - (http://www.dermnetnz.org/bacterial/actinomycosis.html)
- Actinomycosis - (https://www.nlm.nih.gov/medlineplus/ency/article/000599.htm)
What is Actinomycosis?
Actinomycosis is a chronic, rare bacterial infection mostly affecting the face and neck. It can sometimes occur in the chest, abdomen, pelvis and other areas too. This infection is caused by a family of bacteria called Actinomycetaceae. The genus Actinomyces is usually found in the nose, throat, gastrointestinal tract and female genital tract and does not always cause the disease.
Actinomycosis is not a contagious infection, which means that it does spread to other people. The Actinomyces bacterium is anaerobic and cannot survive outside the human body.

How Does Actinomycosis Occur?
Actinomycosis occurs when bacteria get into the skin and tissues. This usually happens after surgery or infection. This can also happen when an intrauterine device (IUD) gets infected. Some of the risk factors for actinomycosis include:
- Dental surgery or other dental trauma leading to poor oral hygiene
- Poor immune system due to medications like immunosuppressants
- Chronic conditions impacting the immune system like diabetes mellitus
What are the Symptoms and Signs of Actinomycosis?
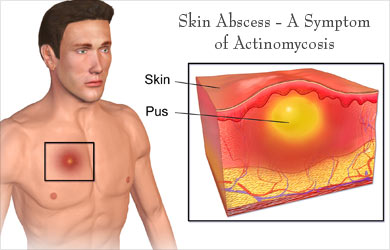
Symptoms of the disease begin with the formation of an abscess and draining sinus tracts, which open on the surface of the skin or membranes to drain the pus. It is often accompanied by fever and weight loss. The affected area is usually red and swollen, which is indicative of inflammation.
How do you Diagnose Actinomycosis?
Actinomycosis is usually diagnosed with a range of blood tests and histopathological tests. Blood tests like CBC (complete blood count) – Lab Test are non-specific; yet have certain markers that point towards bacterial infections. The best diagnostic for actinomycosis is tissue culture by aspirating the abscess or sinus tract (draining pus). This is cultured in the laboratory. If the results indicate gram-positive organisms and sulfur granules, it points towards a strong diagnosis of actinomycosis.
Types of Actinomycosis
Though actinomycosis can affect any part of the body, there are four common types.
The four types are:
- Oral Cervicofacial Actinomycosis - where the infection occurs in the neck, jaw or mouth. In such cases, the infection is usually the result of dental surgery or trauma or jaw injuries. This type is the most common accounting for about 50 to 70% of all actinomycosis cases.
- Thoracic Actinomycosis - where the infection occurs in the lungs and airways. This is usually caused by inhaling contaminated fluids. This type accounts for about 15 to 20% of all cases.
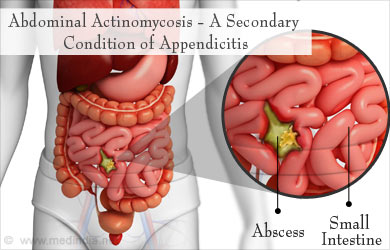
- Abdominal Actinomycosis - where the infection develops in the abdomen. This could be the secondary fallout of a condition like appendicitis, common stomach infections or after accidentally swallowing a foreign body. This type accounts for 20% of all cases.
- Pelvic Actinomycosis - occurs mostly in women when the Actinomyces bacteria spread from the genitals to the pelvic region. In most cases, this infection could be due to long-term use of IUDs. This type accounts for 10% of all cases.
How do you Treat Actinomycosis?
Treatment is long term requiring antibiotics for several months up to one year. Actinomycosis usually responds well to antibiotic regimens. A range of antimicrobial agents can be used like Amoxicillin, Azithromycin and other agents. Initially, antibiotics should be used to cover other bacterial infections found at the site. This could include a combination of amoxicillin with potassium clavulanate. The duration of the antibiotic depends on the severity of the infection.
In some cases, surgical draining of the abscess may be required to avoid further complications. Full recovery is expected after the treatment.
How do you Prevent Actinomycosis?
The best way to prevent actinomycosis is good hygiene practices. Good oral and skin hygiene are best preventives against this infection. Women should maintain vaginal hygiene to avoid pelvic actinomycosis.