- Eric Chung and Gerald B. Brock. Cryptorchidism and its impact on male fertility: a state of art review of current literature. Can Urol Assoc J 2011;5(3):210-4.
- Michael J. Mathers, Herbert Sperling, Herbert Rübben, Stephan Roth. The Undescended Testis: Diagnosis, Treatment and Long-Term Consequences. Dtsch Arztebl Int 2009; 106(33): 527-32.
- Andreas Pettersson, Lorenzo Richiardi, Agneta Nordenskjold, Magnus Kaijser, and Olof Akre. Age at Surgery for Undescended Testis and Risk of Testicular Cancer. N Engl J Med 2007; 356:1835-1841.
- Undescended testicle - (https://medlineplus.gov/ency/article/000973.htm)
- Undescended testicle repair - (https://medlineplus.gov/ency/article/003002.htm)
- What is Undescended testicle? - (http://kidshealth.org/en/parents/cryptorchidism.html#)
- What are Undescended Testicles (Cryptorchidism)? - (http://www.urologyhealth.org/urologic-conditions/cryptorchidism)
- Overview - Undescended testicle - (http://www.mayoclinic.org/diseases-conditions/undescended-testicle/home/ovc-20199764)
- Cryptorchidism - (https://en.wikipedia.org/wiki/cryptorchidism)
- Undescended Testes (Cryptorchidism) - (http://www.stanfordchildrens.org/en/topic/default?id=undescended-testes-cryptorchidism-90-p03081)
- About Undescended testicle? - (http://www.childrenshospital.org/conditions-and-treatments/conditions/u/undescended-testes-cryptorchidism/overview)
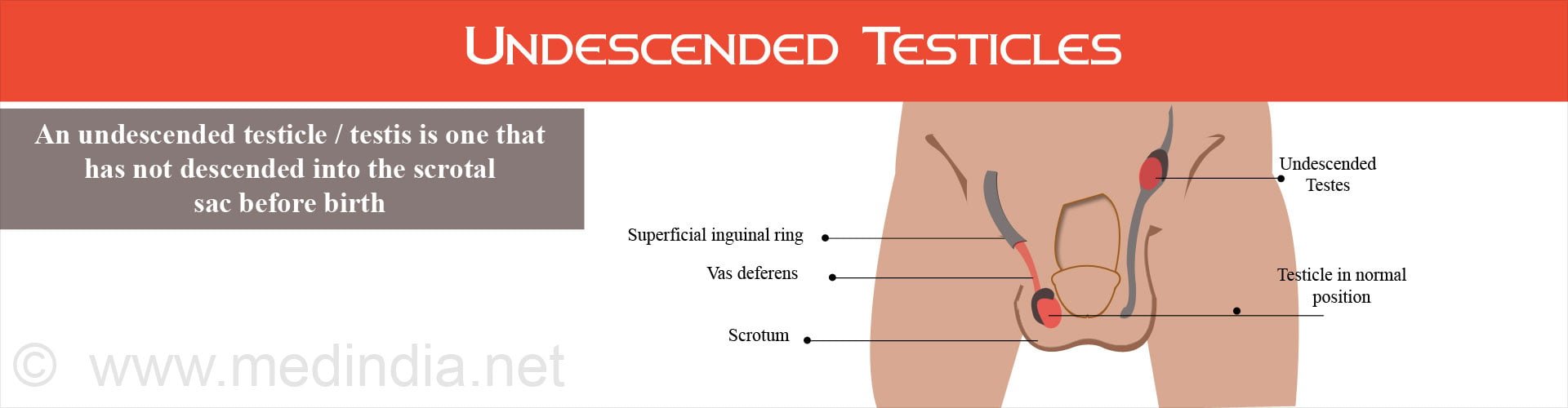
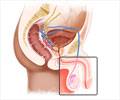
What is an Undescended Testicle?
The testicles are responsible for sperm production in men. Sperm production is best at a temperature 2°C less than the general body temperature of 36.9°C. This is the reason why the testicles are located in a pouch (scrotum) outside the body.
When the fetus develops in the womb, the testicles are initially formed inside the baby’s belly. As the fetus grows, the testicles gradually descend out of the body and reach the scrotum. When this does not happen by the time the baby is born, or is arrested half way, the result is a condition called "undescended testicles” or cryptorchidism.
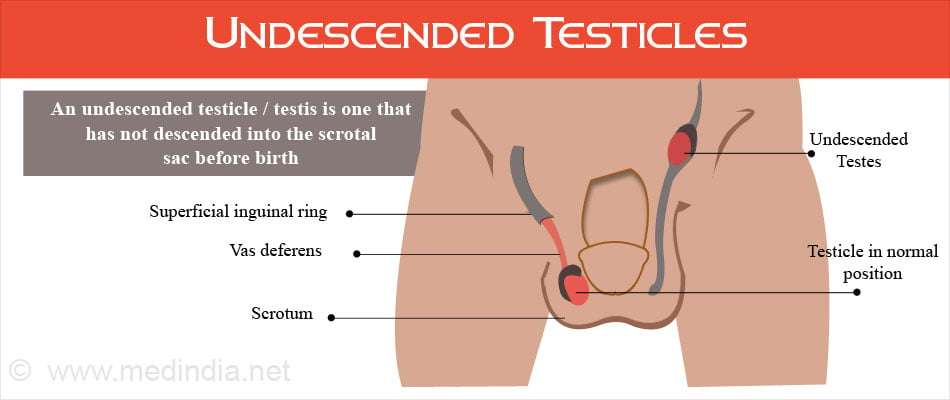
In such cases it is very likely that testicles can descend by themselves within the first few months of life. But this possibility becomes much less after 6 months of age, after which surgery is required to correct it.
There are no symptoms associated with undescended testicles except for not seeing or feeling the testicles in the scrotum.
Facts on Undescended Testicles
- Undescended testicle / testicles are found in 30% of boys born before date (preterm) and around 3% full term boys.
- The testicles descend into the scrotum without any intervention in 75% of boys within around 3 months of life and in 99% of boys within 1 year.
- Testicles cannot be found during the surgery in 5% of males with undescended testicles. This condition is referred to as vanishing testicles.
- Undescended testicles should be differentiated from ascending testicle or retractile testicle. Sometimes, a normally descended testicle at birth might ascend back into the groin at a later date. This is called an “ascending testicle” or an “acquired undescended testicle”. The testicle cannot be easily pulled back into the scrotum. Sometimes the testicle moves back and forth between the scrotum and the groin. This phenomenon is called “retractile testicle”. A retractile testicle is considered normal and is due to a muscle reflex in the scrotum.
What are the Causes and Risk Factors for Undescended testicles?
In most cases, the cause of undescended testicles is not known.
However, some causes and risk factors as to why the testicles do not descend into the scrotum range from -
- Preterm or premature birth
- Low birth weight
- Genetic factors
- Maternal factors (smoking, consuming alcohol or having diabetes mellitus during pregnancy)
- Environmental (persistent exposure to organochlorine compounds, mono-esters of the phthalates)
- Hormonal problems during pregnancy
What are the Complications of Undescended Testicles?
Complications of undescended testicles include the following:
- Infertility: An undescended testicleis exposed to a higher body temperature in the abdomen, which affects sperm production. In later life, these patients have much reduced sperm count and their chances of fathering a child reduce substantially. Infertility is most common in bilateral cases where both the testicles are affected.
- Twisting of Testicles (Torsion): When the testicle is not descended, it is very free to move around itself. This makes it easy to twist and cut off its own blood supply; the result being a loss of the testicle.

- Testicular Cancer: There is a small risk (less than 1 percent) of tumor development in boys born with undescended testicles If the testicle is not brought down into the scrotum by surgery, cancer can develop without being noticed and can become advanced before treatment can be initiated.
- Inguinal Hernia: The person may develop a weak spot in the lower abdomen through which the abdominal lining and even intestines can protrude out.
- Psychological Issues: Boys could feel worry or embarrassment due to an empty scrotum.
How do you Diagnose Undescended Testicles?
A normal physical exam at birth or shortly after by the doctor helps in diagnosing undescended testis. When the sac (scrotum) is poorly formed, one can suspect that the testes have not descended. Also parents may detect it in a similar way when bathing the child.
In 30% of boys, the undescended testicle cannot be located because it is well inside the abdomen or missing or very small. When the testicle cannot be located, it is called “non palpable” or missing.
It could also be that the testicle has followed a non-standard path and descended in an abnormal location outside the scrotum like the lower part of the abdomen, front of the thigh, femoral canal, skin of penis or behind the scrotum. In most cases the testicle is developed but associated with indirect inguinal hernia.
In the case of an undescended testicle that can be located, one can wait for 3-6 months for spontaneous descent. If this does not happen, it is essential to consult a pediatric urologist.
How do you Treat Undescended Testicles?
Hormonal Therapy:
Injecting human chorionic gonadotropin (hCG)or gonadotropin (LH)-releasing hormoneor a combination of the twocan cause hormonal changes that help the testicle to move back to the scrotum. However, the treatment is less preferred when compared to surgery due to lower efficacy.
Surgery - Orchidopexy:
It is recommended to have surgical correction within one year to prevent infertility in later life. The operation is performed under general anesthesia by a pediatric urologist or a pediatric surgeon. A small incision is made in the groin area, the testicle is separated from the tissues around it and the testicle is fixed to the scrotum after achieving enough length. The boy can usually go home the same day and is normal in 1 to 2 days.
Surgery to remove a poorly developed undescended testis from the lower abdomen is performed either with a laparoscope or as an open surgery. A two-staged operation is sometimes needed.
In 5% of boys undergoing the operation, the following complications can occur:
- As a result of damage to the blood supply during the operation, there can be a loss of the testicle.
- When the length of the spermatic cord is not enough and the testicle is under tension, the testicle can go back high again becoming an ascending testicle.
Post-operation: When only one testicle is affected and the surgery is performed at the right time, the success rate is nearly 100% and fertility could even be nearly normal. When both testicles are affected, fertility falls to 65%. Monthly self-examinations must be done to check for possible tumors in both the surgically corrected testicle and in the other one that descended normally.
Another important point to note is that surgery performed before puberty may reduce the risk of developing testicular cancer.