Vanderbilt University Medical Center has become the first hospital in the region to offer a novel approach to cardiac surgery, which doctors believe will change the standard of care for cardiovascular patients.
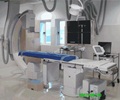
Called the Hybrid OR/Cath Lab, the state-of-the-art operating suite houses all the equipment and monitoring devices necessary to perform open-heart surgeries, like coronary bypass, as well as percutaneous coronary interventions and procedures, including angioplasty and stenting.A major advantage will be the ability to perform an angiogram at the end of routine cardiac surgical cases to make sure grafts are in place and blood is flowing properly. Traditionally, a “before picture” was obtained prior to surgery, but an X-ray study after procedures are completed was not the standard of care.
John Byrne, M.D., likens the Hybrid OR to the change seen in the auto industry after the introduction of safety features like seatbelts and airbags.
“We wear our seat belts every day and have air bags. How often does an air bag deploy? Maybe once or twice in your life. I for one am glad it's there when and if it does deploy. The Hybrid OR/CathLab will catch the rare but very important technical error (if it arises). Just like seat belts and air bags save your life in a car accident.”
Byrne, The William S. Stoney Jr. Professor of Cardiac Surgery and Chair of the Department, said most people had no idea that X-rays of cardiac surgical procedures were not performed post-surgery. He refers to the new operating environment as “sighted” cardiac surgery.
“In virtually every reconstructive procedure in medicine and surgery, the medical team takes a “before” and “after” picture,” said Byrne. “When we put in a central line, nasogastric tube, a chest tube or an endotracheal tube, when your knee or hip is operated on, when you have gall bladder surgery, you get a before and after picture. When you have your heart valve operated on you have a before and after picture (intraoperative echocardiography).
Advertisement
Although Vanderbilt is one of six centers nationally exploring this idea, it is believed to be the first to put the concept to use.
Advertisement
Metry was not hesitant to become a pioneer. His triple bypass surgery was done in the new operating suite.
“The first thing that interested me was the pure science of having the image done in real time,” he said. “They knew that everything was OK when they closed me up. I was also excited that I was getting the A-team.”
Metry, who has a family history of heart disease, was pleased with the entire experience.
“If anyone asked me about the Hybrid OR, I would tell them to do it. You'd want to know as much as possible about the outcome. The doctors can use these outcomes as benchmarks. Measuring outcomes is so important. This is the new direction of medicine.”
And what has been the delay in introducing this medical breakthrough?
Byrne points to the geography of the operating room suites and the cath labs. In most hospitals these facilities are located in separate areas. At Vanderbilt, the OR suites are on the third floor, while the cath labs are on the first floor. Orchestrating the transport of patients requiring both open-heart surgery and interventional procedures is cumbersome and often inefficient, with lag times of up to seven hours. And the need for an X-ray of the procedure would also require transporting patients from the third to the first floor. Finally, if any surgical intervention is needed after an X-ray is obtained, the patient would be transported back to the OR.
Previously at Vanderbilt and still done elsewhere, physicians use what is labeled soft measurements to check a patient's recovery status. These tools include flow probes, EKGs, Echos and ultrasounds which all help determine blood flow. They are not effective when looking at the anatomy of the heart, which is vital when checking for successful grafting and other cardiac procedures, Byrne said.
Another familiar scenario before the Hybrid OR — patients with aortic stenosis or a blockage of the aortic valve with blockage in the right coronary artery; they could have the right coronary artery stented in the cath lab and then be transported to the OR for a minimally invasive valve surgery. It required procedures in two separate locations or at two separate times — both of which require patients to leave and re-enter sterile fields. The Hybrid OR allows them both to be done at the same time, boosting patient safety.
Now that Vanderbilt has opened the Hybrid OR suites, a “one-stop shop” as Byrne refers to it, will create a new model for treating patients.
“The key barrier-to-entry into this new realm has not been equipment or the space. The real barrier-to-entry is collaboration and teamwork between cardiology and cardiac surgery; not just among physicians but also among the OR team and the cath lab team. Dan Brinkman, R.N., director of the cath lab, has been instrumental in building the team.”
At Vanderbilt the teams have been combined to provide a new standard of care, Byrne said. Hybrid procedures will become more common as medical centers begin to see an increase in more complex heart disease patients. The need to image results to measure outcomes will become necessary in order to be more efficient, effective and safe.
“I know this is right,” Byrne said. “I would want it for me or a family member. When you know it's right for the patients, you never lose. This will offer patients, families and referring physicians not only image-guided surgery, but also the ability to provide minimally invasive cardiac surgery combined with percutaneous coronary interventions.”
David Zhao, M.D., assistant professor of Medicine and director of the cardiac catheterization lab and interventional cardiology, agrees.
“First and foremost it provides better care for the patient,” he said. “They receive the best of both worlds through the collaboration of interventional cardiology and cardiac surgery.”
Zhao lauds the new technology, stating that the use of angiography has already proven worthwhile. During a recent bypass, the “after” picture was able to show surgeons that the clip, placed on the graft to stop bleeding, was actually too close to the artery, which comprised the graft and could potentially harm the patient's health.
“The mammary artery has a lot of branches and is the only revascularization conduit that prolongs life,” Zhao said. “In time, that graft would have become occluded and it would not have been discovered for several months or even years if it was not for the Hybrid OR. By doing the post-bypass angiography, you are 100 percent sure the patient has perfect grafts.”
Source-Newswise
SRM