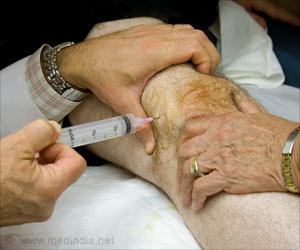
‘Treatment options for hepatitis C have changed dramatically in the last few years. The new medications are effective, but expensive, so it was not clear whether preventing hepatitis C would be as cost-effective or not.’
Tweet it Now
"The new medications are very effective, but they are also very expensive, so it was not clear whether preventing hepatitis C would be as cost-effective as it was just a few years ago" said the study's senior author, Dr. Ahmed Bayoumi. "Our analysis also incorporated the speed at which hepatitis C drugs would be rolled out to people who inject drugs and the risk of reinfection among people who continue to inject." The study results were published today in the journal Addiction. Dr. Bayoumi, a physician at St. Michael's Hospital and a researcher in its Centre for Research on Inner City Health, as well as an adjunct scientist at the Institute for Clinical Evaluative Sciences, said there was an 86 percent chance that one or more supervised injection facility would be cost-effective in Toronto and a 90 percent chance in Ottawa.
He said the conclusions may be conservative, noting that the operating costs used in the analysis were based on the facility being located in its own freestanding building--like Insite in Vancouver, the only legal supervised injection facility in North America. However, recent recommendations have suggested incorporating supervised injection services into existing health facilities, which could be considerably less expensive.
Dr. Bayoumi also stressed that it would be necessary to evaluate any facilities to determine if the reduction in needle sharing rates in Toronto and Ottawa would be the same as was observed in Vancouver (68 percent).
In the 2012 report that recommended supervised injection facilities for Toronto and Ottawa, Dr. Bayoumi and co-principal investigator Dr. Carol Strike of the University of Toronto, said such facilities could prevent HIV and hepatitis C infections and could also reduce public drug use. That report was based on a four-year study, believed to be the largest of its kind.
Advertisement
However, if Toronto and Ottawa proceed, the researchers recommended multiple sites, not a single, central location like Insite. Drug use is dispersed in Ontario's two largest cities, unlike Vancouver where it is concentrated in the Downtown Eastside. In addition, people who use drugs indicated they did not want a single facility that could become a focus of opposition. Community members consulted by the researchers also preferred multiple locations spread out across each city to minimize possible impacts on local neighborhoods.
Advertisement