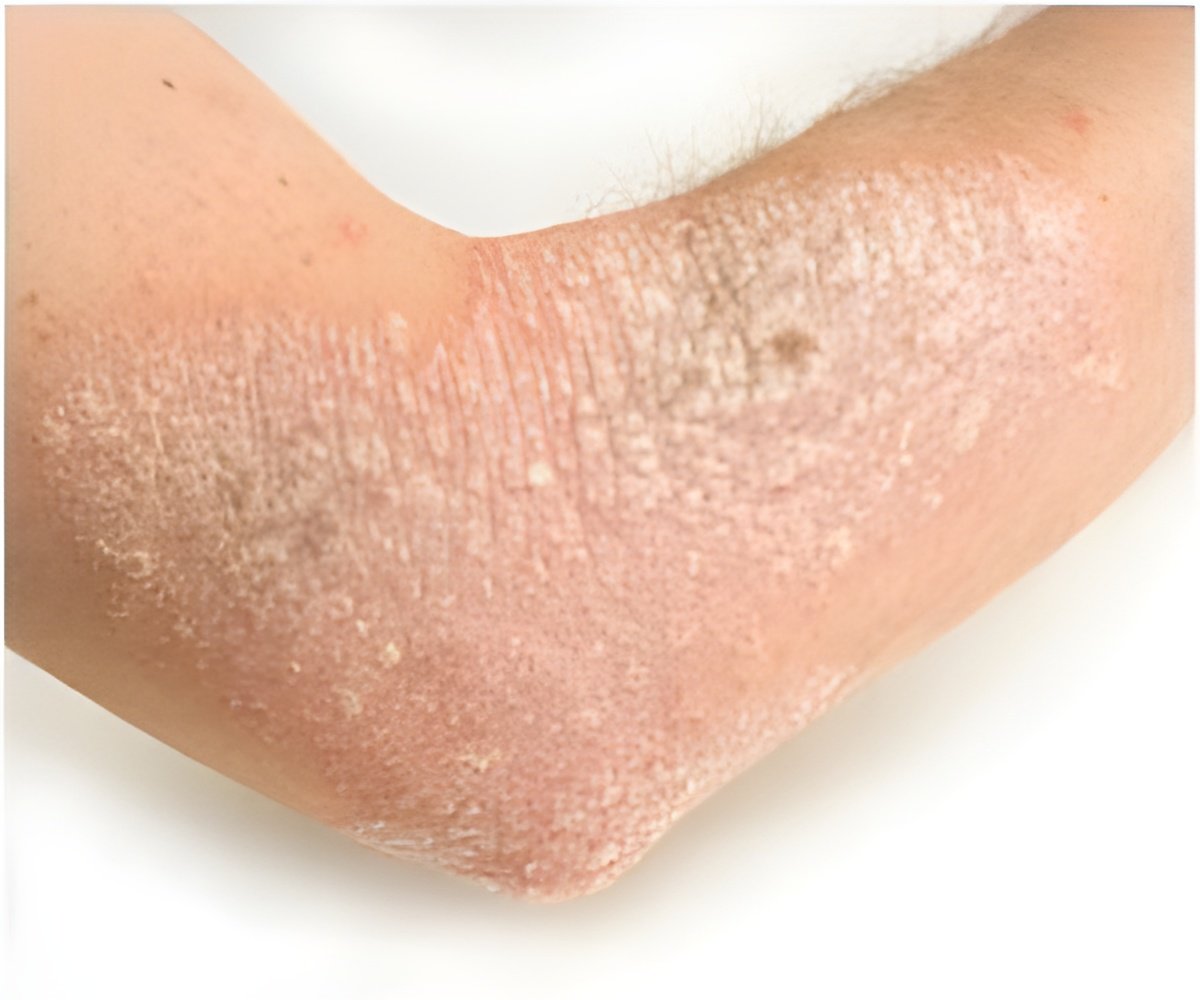
Eczema is also related to, and can sometimes cause asthma, a potentially deadly immune dysfunction.
Pharmaceutical scientists at OSU found in laboratory studies that eczema can be triggered by inadequate Ctip2, a protein and master regulator that affects other genetic functions.
They have identified two ways in which improper function of Ctip2 can lead to eczema.
In a recent publication, they found that Ctip2 controls lipid biosynthesis in the skin, the fats that are needed to help keep skin healthy and hydrated. In the new study, they discovered that Ctip2 suppresses TSLP, a cytokine protein produced by skin cells that can trigger inflammation.
Levels of this inflammatory TSLP, which is ordinarily undetectable in human skin, were found to be 1,000 times higher in laboratory animals that had been genetically modified to have no Ctip2 production in their skin.
Advertisement
"At the same time this can allow unwanted formation of proteins that trigger inflammation. The skin's ability to resist inflammation is going down just as the amount of inflammation is going up, and the underlying reason is that Ctip2 is not doing its job.
Advertisement
Atopic dermatitis is associated with a dysfunctional immune response, but researchers have never understood the underlying cause. Existing treatments use moisturizers to try to protect skin, and in difficult cases powerful steroid drugs can help, but they often have significant unwanted side effects, especially in long-term use.
"With a better understanding of just what is causing eczema on a genetic basis, we should be able to personalize treatments, determine exactly what each person needs, and develop new therapies," Indra said.
"This might be with topical compounds that increase Ctip2 expression in skin cells, or customized treatments to restore an individual person's lipid profile. In the future, systemic epigenetic modification might even be possible," he said.
According to him, the creation at OSU of the laboratory model to study this issue is also of considerable importance, and there's evidence that it could be used to screen for drugs with potent anti-inflammatory activities.
The study has been recently published in PLoS ONE.
Source-ANI