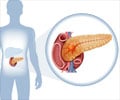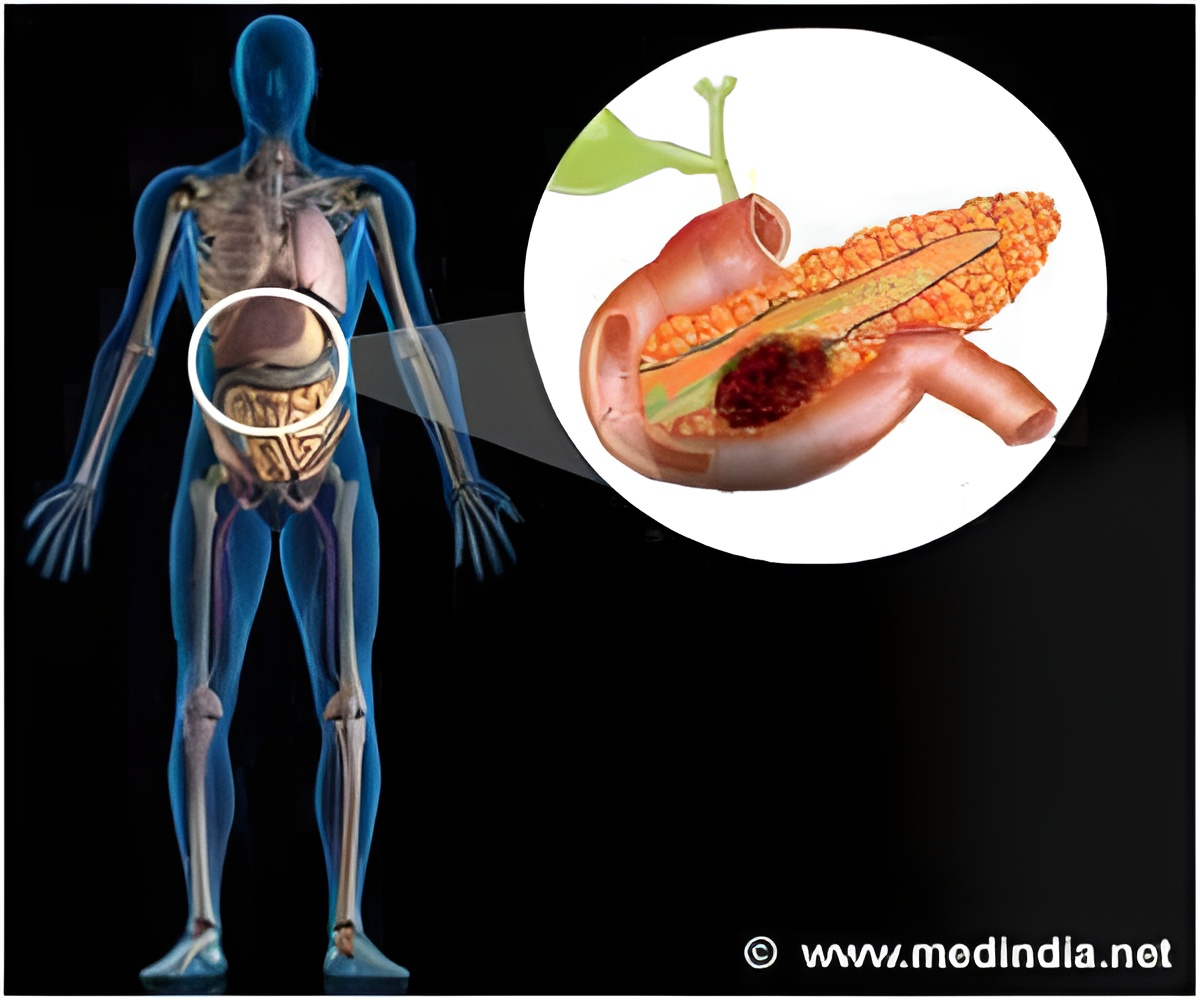
Pancreatic cancer is one of the most deadly types of cancer, mostly because of its aggressiveness and its ability to suppress the cancer fighting properties of the immune system. Essentially, all pancreatic cancer cells harbor a mutation in the KRAS gene. Two teams of researchers looked to see how mutated KRAS gives pancreatic cancer its distinguishing properties.
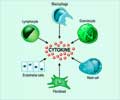
Using mouse models of pancreatic cancer, the two groups each found that mutated KRAS triggers pancreatic tumors to express a protein called GM-CSF. They also discovered that tumor-derived GM-CSF recruits immature immune cells to the areas surrounding the tumor and then coaxes those cells to mature into so-called myeloid-derived suppressor cells, which suppress the surveillance function of other immune cells that normally seek out and destroy foreign and malignant cells. In this way, pancreatic cells escape being seen by the body's immune system and are free to grow and divide. Blocking GM-CSF production, however, inhibited myeloid-derived suppressor cells and enabled the immune system to halt tumor development.
The researchers also showed that human pancreatic cancer cells prominently express GM-CSF, indicating that the findings could lead to new treatments for patients. "Our studies suggest a therapeutic strategy by which the antitumor properties of a patient's immune system can be restored," says Dr. Dafna Bar-Sagi of the NYU School of Medicine, who is the senior author of the second paper.
Source-Eurekalert