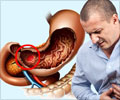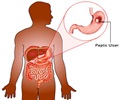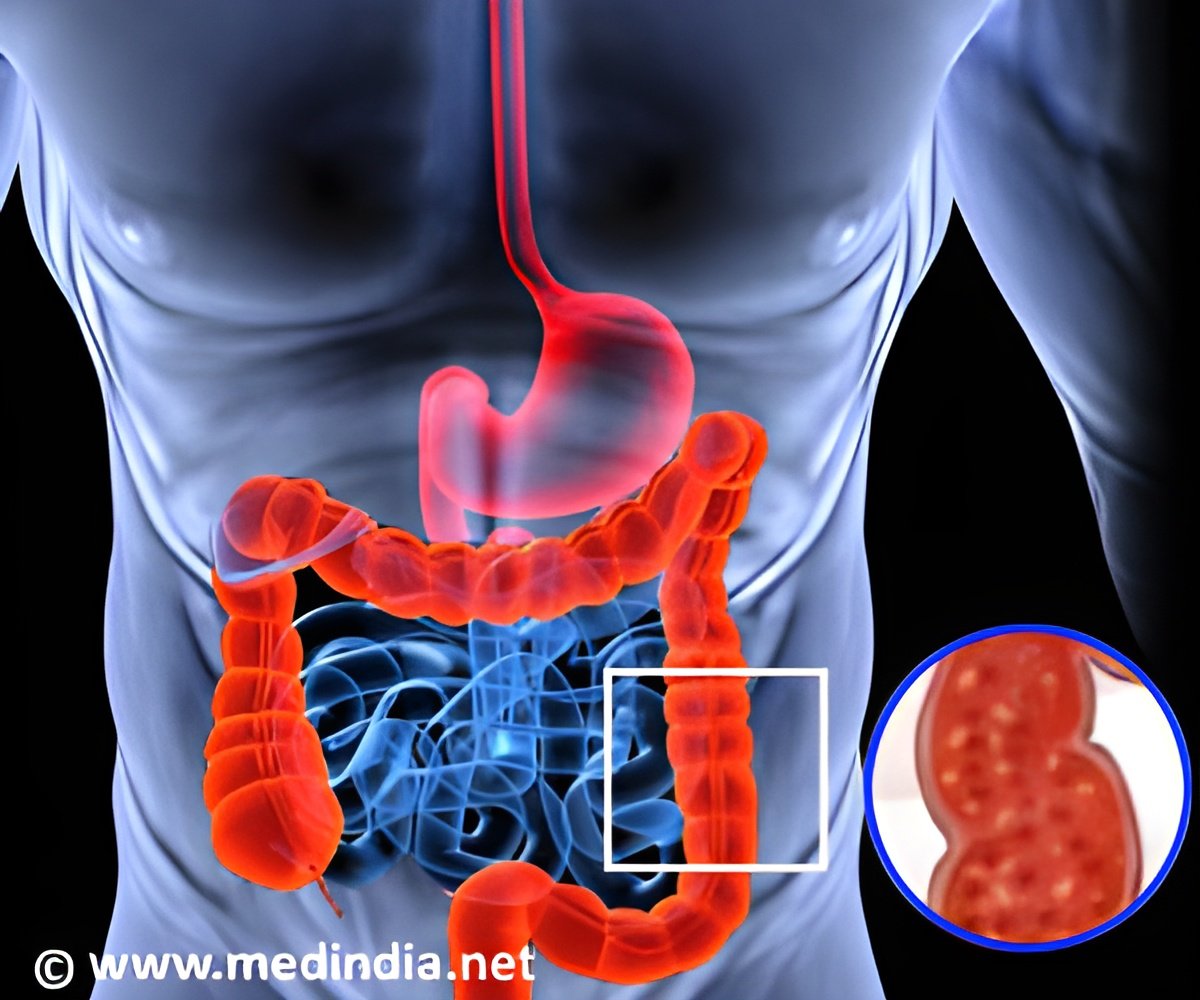
Conventional treatment of GI defects is with surgical management, which is associated with significant morbidity and mortality. Technological advances in endoscopic devices have allowed for endoscopic closure of GI defects. Endoscopic therapies include placement of self-expandable metal stents (SEMSs) and application of clips and sealants, all of which have proven their utility in different clinical scenarios with varying degrees of success. The most common endoscopic approach for treatment of GI defects before the over-the-scope clip was the use of temporary SEMSs.
A large case series reported a success rate as high as 75 percent with SEMSs; however, this practice was associated with a high rate of adverse events (46 percent). The OTSC provides more durable closure than standard clips because of its wider mouth and ability to grasp larger amounts of tissue. In addition, full-thickness closure is achievable because of greater compressive force. The current study is the largest to-date to assess outcomes of OTSCs in the management of GI fistulae, perforations and leaks.
"The primary goal of this study was to describe a large, international, multicenter experience with OTSCs for the management of GI perforations, fistulae and anastomotic leaks and to determine the overall success of GI defect closure. Secondary goals were to determine success rate by type of defect and type of therapy, primary vs. rescue, and to determine predictors of OTSC success," said study lead author Yamile Haito-Chavez, MD, Johns Hopkins University, Baltimore, Maryland. "Our study found that long-term success was achieved in 60.2 percent of patients. The rate of successful closure of perforations was 90 percent, closure of leaks was 73.3 percent and closure of fistulae was 42.9 percent. Long-term success was significantly higher when OTSCs were applied as a primary therapy."
A retrospective review of consecutive patients who underwent attempted OTSC placement (either as primary or rescue therapy) for the indication of GI leak, fistula or perforation at 16 academic centers in the United States, The Netherlands, Germany, Italy, and Chile was conducted between May 2006 and November 2012. Patients were identified by using endoscopic databases at each institution. Anastomotic leak was defined as disruption at a surgical anastomosis resulting in a fluid collection with or without evidence of extravasation of contrast medium on radiologic evaluation. Fistula was defined as abnormal communication between two epithelialized surfaces. Perforation was defined as an unintentional, acute iatrogenic, full-thickness defect in the GI tract. The main outcome measurement was the long-term success of the procedure.
A total of 188 patients (108 fistulae, 48 perforations, 32 leaks) were included. Long-term success wasachieved in 60.2 percent of patients during a median follow-up of 146 days. The rate of successful closure of perforations (90 percent) and leaks (73.3 percent) was significantly higher than that of fistulae (42.9 percent). Long-term success was significantly higher when OTSCs were applied as primary therapy (primary 69.1 percent vs. rescue 46.9 percent). On multivariate analysis, patients who had OTSC placement for perforations and leaks had significantly higher long-term success compared with those who had fistulae.
Advertisement
Advertisement