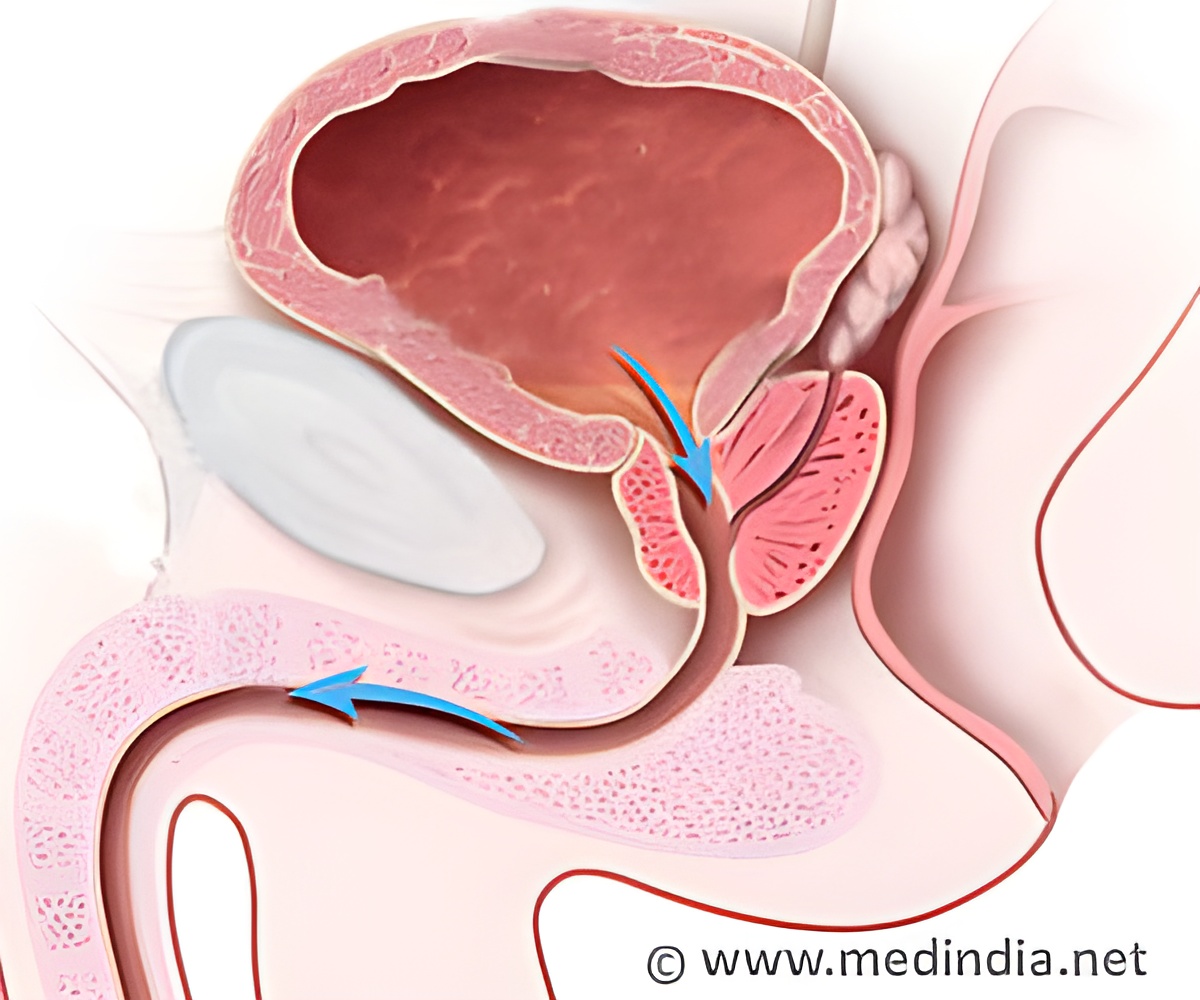
‘When genomic fingerprinting is performed on only a single prostate tumor sample, a smaller but more aggressive tumor could potentially be missed, suggested a study.’
Tweet it Now
The finding underscores the importance of new evidence that prostate tumors can be genetically different within an individual patient, which carries important implications for patients and oncologists.For the study, “Intratumoral and Intertumoral Genomic Heterogeneity of Multifocal Localized Prostate Cancer Impacts Molecular Classifications and Genomic Prognosticators,” the team used next-generation sequencing techniques to genotype prostate tumors from four men who underwent radical prostatectomy at Roswell Park. They also examined public data from the Cancer Genome Atlas to confirm their findings.
“We examined the molecular composition of heterogeneous cancerous tumors in a patient’s prostate. We found a lot of genetic differences among these tumors, and concluded that information from a single cancer biopsy is not sufficient to guide treatment decisions,” said Dr. Heemers. “Precise treatment is more complicated and the findings demonstrate a weakness in current genetic fingerprinting in prostate cancer.”
“High risk prostate cancers differ genetically among patients, among the different tumors within an individual patient and even within different sections of a single tumor,” said Dr. Mohler. “Clinicians need to be careful about using the information from a gene-based test, because the analysis may not have been performed on the most aggressive portion of a man’s prostate cancer.”
In “Disrupting the Status Quo in Prostate Cancer Diagnosis,” an editorial published in the same journal, Alastair David Lamb, of Cambridge University Hospitals, and co-authors write, “Several aspects of this study are impressive. [The authors] addressed an important clinical and molecular question: What effect does tumor heterogeneity have on decision making in prostate cancer, specifically, with respect to molecular taxonomies of the disease?”
Advertisement
Source-Newswise



![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)









