S. Matthijs Boekholdt, M.D., Ph.D., of the Academic Medical Center, Amsterdam, the Netherlands, and colleagues conducted a meta-analysis to assess whether among patients receiving statins, non-HDL-C and apoB were more strongly associated with the risk of future cardiovascular events than LDL-C. The study included individual patient data from randomized controlled statin trials in which conventional lipids and apolipoproteins were determined in all study participants at baseline and at 1-year follow-up. The researchers identified 8 trials, published between 1994 and 2008, that met criteria for inclusion in the meta-analysis. The trials included individual patient data for 62,154 patients.
A total of 38,153 study participants were randomized to a statin group and had a complete set of lipid and apolipoprotein levels during statin treatment available. Among these individuals, a total of 158 (0.4 percent) developed a fatal heart attack and 1,678 (4.4 percent) developed a non-fatal heart attack during follow-up. Fatal other coronary artery disease occurred in 615 study participants (1.6 percent) and fatal or nonfatal stroke occurred in 1,029 study participants (2.7 percent). A total of 2,806 participants (7.4 percent) were hospitalized for unstable angina. A total of 6,286 major cardiovascular events occurred in 5,387 study participants (event rate 14.1 percent).
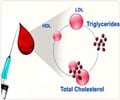
Analysis of the data indicated that among statin-treated patients, levels of LDL-C, non-HDL-C, and apoB were each strongly associated with the risk of major cardiovascular events, but non-HDL-C was more strongly associated than LDL-C and apoB. Also, changes in non-HDL-C explained a larger proportion of the atheroprotective effect of statin intervention than did LDL-C and apoB.
"Given the fact that many other arguments for the clinical applicability of non-HDL-C and LDL-C are identical, non-HDL-C may be a more appropriate target for statin therapy than LDL-C," the authors conclude.
Source-Eurekalert