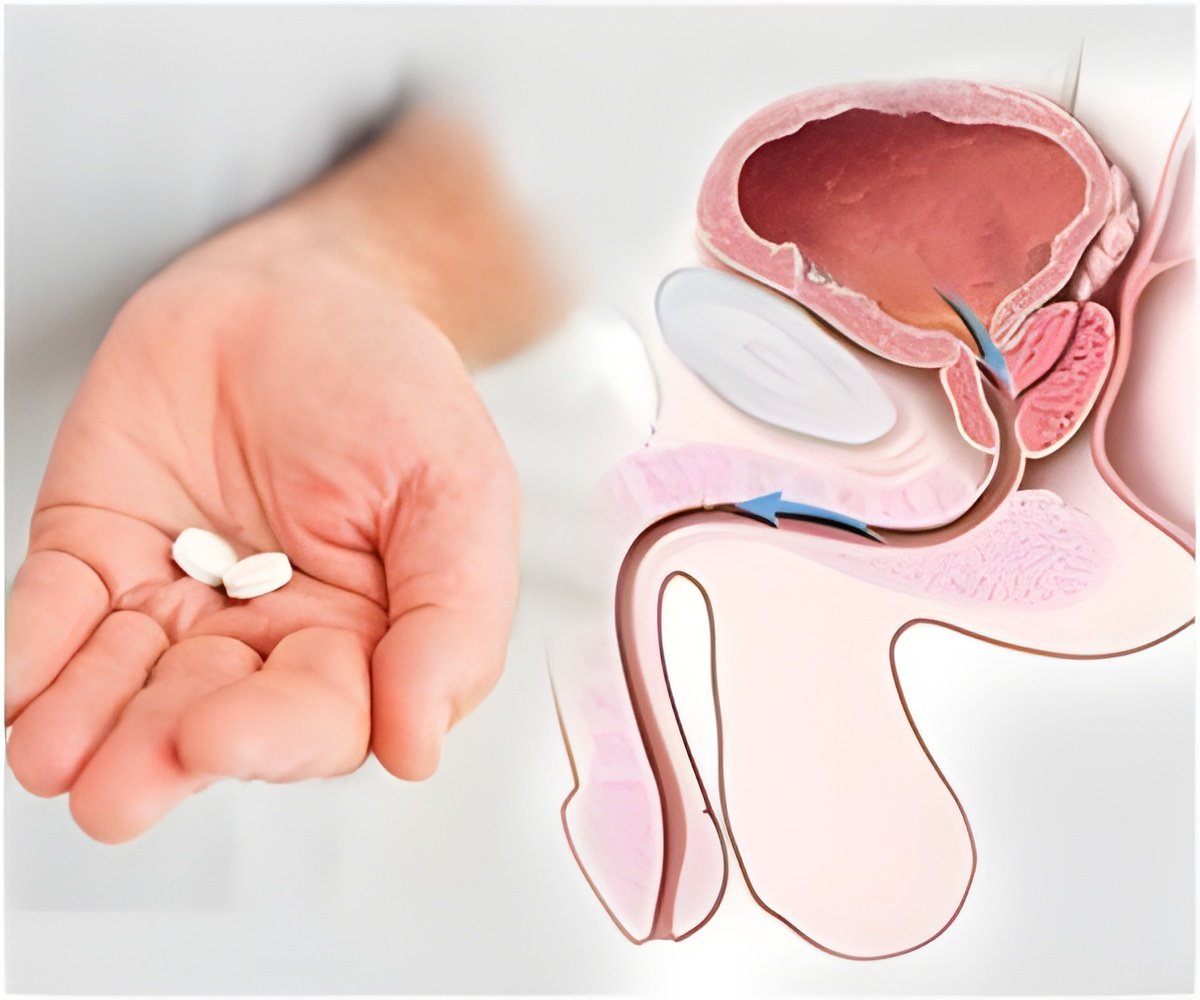
The Task Force last published recommendations on prostate cancer screening in 2008. At the time, researchers concluded that there was no evidence to support PSA testing for men over the age of 75. An independent panel of experts reviewed evidence published since 2008 and concluded that the harms of PSA testing outweigh the benefits regardless of age. The Task Force considers health benefits and harms, but not costs, when developing recommendations.
The primary goal of prostate cancer screening programs is to save lives and prevent symptomatic disease. The Task Force considered two major trials of PSA testing in asymptomatic men to assess the life-saving benefits of PSA testing. The first trial, conducted in the U.S., did not demonstrate any prostate cancer mortality reduction as a result of screening. The second trial, conducted in seven European countries, found a reduction in prostate cancer deaths of about one death prevented per 1,000 men screened in a subgroup of men aged 55 to 69 years, mostly in two countries. Five of the seven countries reporting results did not find a statistically significant reduction in deaths.
Strong evidence shows that PSA screening is associated with significant harms. Nearly 90 percent of men with PSA-detected prostate cancer undergo early treatment with surgery, radiation, or androgen deprivation therapy. Evidence shows that up to five in 1,000 men will die within one month of prostate cancer surgery and between 10 and 70 men will survive, but suffer life-long adverse effects such urinary incontinence, erectile dysfunction, and bowel dysfunction.
According to William J. Catalona, M.D., Medical Director of the Urological Research Foundation and author of an accompanying editorial, the Task Force recommendation has underestimated the benefits and overestimated the harms of prostate cancer screening. He and his co-authors argue that the Task Force -- whose panel does not include urologist or cancer specialists -- largely bases its recommendations on flawed studies with inadequate follow up time. In addition, the Task Force recommendations focus on mortality and do not take into consideration the substantial illness related to living with advanced cancer.
Editorial co-author, Dr. Henry Lynch, Director of the Hereditary Cancer Center at Creighton University, adds that the Task Force recommendations also leave out high-risk populations and younger men. The authors express concern that the new recommendations will take Americans back to an era when prostate cancer was often discovered at advanced, incurable stages.
Advertisement
Yet, according to Otis W. Brawley, MD, MPH, Chief Medical Officer of the American Cancer Society, and author of a second accompanying commentary, overdiagnosis makes screening seem to save lives when it truly does not. Many men are diagnosed with prostate cancer that may never have progressed within their lifetime. Yet because they were screened and treated, they think screening saved their lives.
Advertisement
In October 2011, the Task Force posted its draft recommendations for public comment. At the time, the Task Force had given PSA screening a grade “D,” meaning that physicians should not offer the test because the harms outweigh the benefits. Many people who commented on the recommendations urged the Task Force to change the recommendation to a grade “C,” meaning physicians could provide the test to patients who request it. However, no new evidence was presented. The recommendation remains unchanged.
While the recommendation clearly states that physicians should not offer PSA screening, the Task Force says it leaves the ultimate power in the hands of the health care providers.
“The USPSTF recognizes that clinical, policy, and coverage decisions involve more considerations than evidence alone,” said Task Force Chair, Virginia A. Moyer, MD, MPH of Baylor College of Medicine in Houston, TX. “Clinicians and health care providers should understand the evidence but individualize decision-making to the specific patient or situation.”
Source-Eurekalert



![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)