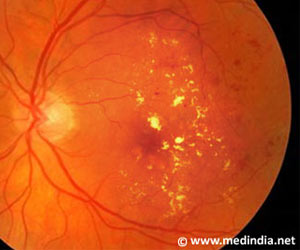
‘An association between a defective myogenic response and early, accelerated development of retinopathy in patients with type 1 diabetes has been identified by researchers.’
Tweet it Now
Currently, there are no treatments for diabetic retinopathy beyond controlling blood sugar and blood pressure levels. The new vessels of proliferative retinopathy can be treated with laser techniques, often at the expense of a portion of the retina.Researchers from Massachusetts Eye and Ear and Schepens Eye Research Institute have shown an association between a defective myogenic response - the regulatory increase or decrease in blood pressure to keep blood flow within the vessels of the retina constant - and early, accelerated development of retinopathy in patients with type 1 diabetes.
These findings are published in Investigative Ophthalmology and Visual Science. The researchers identified one mechanism to explain why some patients develop diabetic retinopathy sooner than others. Furthermore, the findings provide a target for future study, which may lead to therapies to delay or prevent the development of accelerated onset diabetic retinopathy.
"In patients with a normal myogenic response, the retinal vessels constrict when increased pressure arrives, to maintain constant blood flow and avoid damage to the smaller vessels in the retina," said Mara Lorenzi, senior scientist at Massachusetts Eye and Ear/Schepens Eye Research Institute and a professor of ophthalmology, part-time at Harvard Medical School. "But we saw that, in about half of the diabetic patients in our study, the vessels did not constrict. In fact, paradoxically, some patient' vessels dilated, and the blood flow to the retina was increased. This becomes a mechanism of damage for the small vessels, because these tiny, delicate capillaries are exposed to a big flow of pressure that can lead to the little hemorrhages and fluid leakage that are characteristic of diabetic retinopathy."
The study included a small prospective study, in which the researchers closely followed 17 patients with type 1 diabetes whose myogenic responses had been measured four years prior. In approximately half of those patients, the researchers had observed defective myogenic responses. Five out of seven patients with defective myogenic responses developed accelerated diabetic retinopathy. The study also included a different group of patients with type 1 diabetes who had just developed retinopathy. Among these patients, the defective myogenic response was found only in those in whom retinopathy had appeared after a short duration of diabetes (fewer than 15 years of diabetes).
Advertisement
"Now, we have a target to be investigated for the development of drugs or interventions to halt or stall the onset of clinical retinopathy," Dr. Lorenzi said.
Advertisement