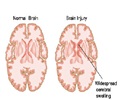
More than 35,000 Americans are diagnosed with a cancerous brain tumor every year, according to the U.S. National Cancer Institute. Prognosis for glioma is particularly dismal, with adults aged 45-55 having a six percent chance of surviving five years after diagnosis. Only three percent of those over 55 are likely to be alive at the five-year mark. Gliomas are malignant tumors of the neuroglia, or glial cells—the glue that holds neurons in the brain and spine together and keeps them healthy. When these cells do not die as they are naturally designed to, or when they begin to grow out of control, they are considered malignant. The general line of treatment for these invasive brain tumors is surgery, radiation and chemotherapies, but gliomas are notorious for recurring after treatment.
Novel brain cancer treatments for glioma provide a more potent and targeted kill, which could significantly improve patient survival rates. In an effort to find an imaging method to compliment these treatments, researchers tested a combination of positron emission tomography (PET)—a molecular imaging technique that provides information about biological processes—and an amino acid imaging probe targeting the increased protein transport of these cancerous brain cells. Researchers evaluated the ability of this combination to inform clinicians about how a specific antiangiogenic therapy (used to halt the growth of cancer) was performing after it was administered to patients. Results showed that amino-acid PET was effective for monitoring their treatment, and in record time—just two weeks after the initiation of therapy.
Upon injection, the amino-acid analog is transported into brain cells. Positron signals emitted from the imaging biomarker are then picked up by a PET scanner. Clinicians can see where cancers are still active because malignant cells take up more of this protein than healthy cells. Amino-acid PETimaging provides visual evidence, within a few weeks, of whether aggressive treatments are working because "hot-spots" of high amino-acid uptake in cancer cells on previous scans diminish dramatically in scans after successful therapy.
For this National Institutes of Health study, 30 patients with recurrent high-grade gliomas underwent F-18-FDOPA PET scans immediately before treatment with bevacizumab combination therapy and then again at two and six weeks after therapy. PET scans were compared to MRI for treatment response. Participants who responded positively to treatment, as evidenced with F-18-FDOPA PET imaging, lived three times longer than those who responded poorly (from the start of treatment).
"This technique still needs FDA approval for clinical use, but all of this is in the works," says Chen. "If this were made readily available it would provide clinicians a powerful tool to help patients with this deadly disease."
Advertisement
Source-Eurekalert