‘Physicians in pediatric intensive care units are not using the newest guidelines to diagnose acute kidney injury in critically ill children, a practice that could affect their patients' long-term health.’
Tweet it Now
A pediatric critical care physician who focuses on acute kidney
injury, Amanda Hassinger surveyed colleagues in her field on practice
patterns related to the diagnosis and treatment of AKI. The study was reported in a recent paper in the journal Pediatric Critical Care Medicine.
"What we found was pretty surprising. It was scarier than I thought in terms of how aware other physicians in my field are to the new guidelines for treatment of AKI and the new methods to diagnosis earlier and more effectively," said Hassinger, lead author on the paper, published in the journal's August issue.
She wrote it while working on her master's degree in epidemiology/clinical research in UB's School of Public Health and Health Professions. Hassinger has been an attending physician in the Division of Critical Care at Women & Children's Hospital of Buffalo, and is also an assistant professor of pediatrics in UB's Jacobs School of Medicine and Biomedical Sciences and a member of UBMD Pediatrics.
Hassinger and her co-authors surveyed 170 pediatric critical care physicians from academic centers, the Pediatric Acute Lung Injury and Sepsis Investigators network and the pediatric branch of the Society of Critical Care Medicine.
Advertisement
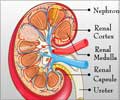
The problem with serum creatinine as a test for renal function, Hassinger says, is that it is not effective in children for detecting AKI. It can be affected by several other factors, including nutrition and muscle mass. Several new biomarkers have been discovered that aid in the diagnosis of AKI.
Advertisement
"I wasn't surprised that the newer tests aren't being used, because they do cost a lot of money and require special machinery," Hassinger says. "But what really upset me was that physicians were happy with the status quo and weren't looking for a better biomarker for this critically important condition. The existing biomarkers are inadequate. That was disappointing."
AKI occurs most frequently in patients who are already in the hospital. It can be caused by a number of health conditions, including sepsis, shock, trauma, exposure to medications that affect the kidneys, or major surgery.
What's more, according to the National Kidney Foundation, one episode of AKI increases a patient's chances of developing other health problems - such as kidney disease, stroke or heart disease - later in life. In fact, Hassinger said, data now show that children who experience a single episode of AKI in the ICU have a 50% to 75% chance of having renal insufficiency for the rest of their life.
"It's an important but silent issue that needs more attention," she says. "The kidneys are a very vulnerable set of organs and they're important to overall balance in the body, so we should be paying more attention to them than we do. Somebody has to fight for the little beans."
"This study gives us an important picture of what practice looks like in pediatric ICUs, so that we can understand what is missing," said Jo Freudenheim, chair of epidemiology and environmental health in UB's School of Public Health and Health Professions, and a co-author on the paper. "We can now start to make renewed efforts to change practice and to improve care."
Hassinger has an idea why AKI often goes underappreciated. "The kidneys are extremely resilient, and children are resilient, so even if you have the worst stage of acute kidney injury, despite the physician, the kidneys and the patient get better. There's not as much urgency to diagnose it and call it the right name because most of the time, no matter what name you call it, kids will bounce back pretty well," she said.
Toward that point, the researchers' survey asked physicians if they were aware that AKI independently has increased morbidity and mortality. 12% of the respondents - a particularly high number, Hassinger says - said either no or that they were unsure.
Hassinger was also surprised to learn that just one-third of the PICU physicians surveyed said they refer a child who has AKI to a kidney specialist once the patient is discharged from the intensive care unit. That means that two-thirds of the respondents reported either rarely or never offering referrals.
"So these patients go unmonitored for periods of time until the kidney issues manifest when they're teenagers and they get an infection or another injury that knocks out the kidneys completely, and then they're in renal failure at 18," Hassinger said.
Hassinger is partnering with a colleague at Cincinnati Children's Hospital Medical Center for a second survey that will take a closer look at the relationship between fluid overload and acute kidney injury in ICU patients. Fluids, given through IVs, are used regularly in hospitalized children. Fluid overload can cause organs to fail, Hassinger said, explaining why that's another area of current medical practice that needs better scrutiny.
Source-Eurekalert