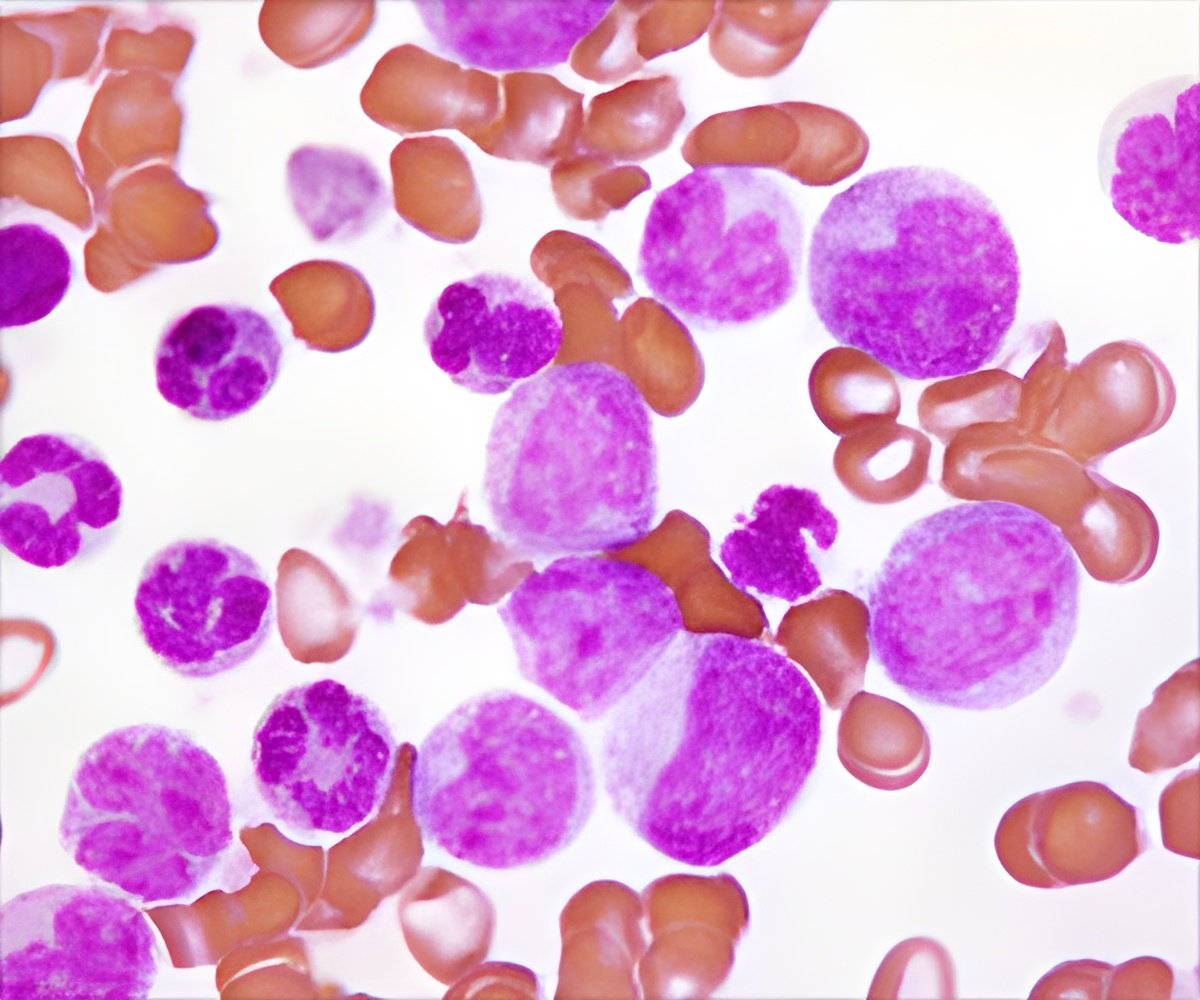
ALL is the most common childhood cancer. The research focused on a subtype of ALL known as Philadelphia chromosome-like ALL (Ph-like ALL). In 2009, St. Jude scientists, working with the Children's Oncology Group (COG), were among the first to describe the Ph-like ALL subtype in children. The present study found the prevalence of Ph-like ALL increases with age and that the subtype is associated with poor survival. The discovery followed a detailed genomic analysis of 1,725 patients ages 1 to 39 with the most common form of ALL, which involves white blood cells known as B cells and is called B-ALL.
Researchers also used next-generation sequencing to identify the genetic alterations that give rise to Ph-like ALL, including some involving genes not previously linked to cancer. The results highlight the genetic diversity of Ph-like ALL, but also demonstrate that alterations affect a limited number of biological signaling pathways. Those pathways regulate genes controlling cell growth and proliferation, which are disrupted in cancer.
The findings, combined with earlier work from St. Jude and other institutions, laid the foundation for clinical trials to determine whether drugs called tyrosine kinase inhibitors (TKIs) could help improve patient outcomes. A nationwide study meant to answer that question in children is scheduled to begin later this year or early in 2015. By targeting enzymes known as kinases, TKIs work more precisely than chemotherapy drugs to kill cancer cells.
"We showed that Ph-like ALL is a common disease that spans the age spectrum, and we identified new genomic alterations that converge on a handful of signaling pathways that are vulnerable to treatment with tyrosine kinase inhibitors," said corresponding author Charles Mullighan, M.D., MBBS(Hons), a member of the St. Jude Department of Pathology. "The findings lead the way for clinical trials that could help to transform the outlook for patients regardless of age."
TKIs, including drugs like dasatnib and imatinib, are widely used to treat other types of leukemia that are more common in adults. The drugs have also been used in a small number of patients with Ph-like ALL. This study reports the experiences of eight such patients, including seven children who were treated at different medical centers. All had leukemia that persisted despite chemotherapy. Each patient enjoyed a dramatic, immediate benefit when a TKI was added to the treatment regime. Five patients remain in remission with no detectable cancer, one for more than a year.
Advertisement
Ph-like ALL is named for a chromosomal rearrangement known as the Philadelphia (Ph) chromosome, which is associated with a different subtype of ALL. Both Ph-positive and Ph-like subtypes of ALL share similar patterns of gene expression, but patients with Ph-like ALL lack the fusion of the BCR and ABL1 genes that is a feature of Ph-positive ALL.
Advertisement
Regardless of their age, patients with Ph-like ALL were less likely than other B-ALL patients to be alive and cancer free five years after their disease was discovered. Overall survival for children, adolescents and young adults with Ph-like ALL was 62 percent compared to 91 percent for other B-ALL patients of the same age. Leukemia-free survival was about 47 percent for patients with Ph-like ALL and about 83 percent for other patients.
The search for the genetic changes that give rise to Ph-like ALL included whole genome sequencing of 42 patients plus additional sequencing, including of RNA from the leukemic cells of 136 patients. The genome is the complete set of instructions needed to assemble and sustain life. It is encoded in the DNA molecule carried in almost every cell. RNA sequencing provides a snapshot of gene activity in cells.
Researchers found that 91 percent of patients with Ph-like ALL had chromosomal rearrangements or other genetic alterations that activate cytokine receptor or kinase signaling. An analytic tool called CICERO, which was developed by St. Jude researchers, played a key role in identifying the changes. Kinases are enzymes that serve as on-off switches in cells. Cytokine receptors regulate how cells respond to growth factors called cytokines.
"We identified several new subgroups of Ph-like ALL that were distinguished by the type of cytokine receptor or kinase gene alteration," said Kathryn Roberts, Ph.D., a St. Jude postdoctoral fellow. She and Yongjin Li, Ph.D., a St. Jude Department of Computational Biology research scientist, are the paper's co-first authors.
Evidence suggests that several of the newly identified Ph-like ALL subtypes are vulnerable to TKIs and other targeted therapies. For example, about 12 percent of patients had rearrangements involving the genes ABL1, ABL2, CSF1R and PDGFRB, which are known to respond to dasatnib and related TKIs.
Numerous other Ph-like ALL patients had gene rearrangements involving JAK2, EPOR and other genes that can be targeted by the drug ruxolitinib. Approved for use against a bone marrow disorder, ruxolitinib is being studied for treatment of a variety of cancers.
The research was part of the Pediatric Cancer Genome Project, a collaboration of St. Jude and Washington University School of Medicine in St. Louis that uses next-generation genome sequencing technology to improve understanding and treatment of some of the most aggressive and least understood childhood cancers. The complete normal and tumor genomes of 700 young cancer patients have been sequenced as a result of the project, which began in 2010.
Source-Eurekalert