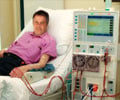
Hemodialysis is resorted to when the kidney function of filtering the blood and producing urine goes down below 10 to 15 percent or when the kidney does not function at all (called the end-stage renal disease or ESRD). This is a therapy where the blood is removed from the body and filtered through an ‘artificial kidney’ (a machine that helps to purify the blood) and then the ‘purified’ blood is returned to the body. The therapy helps in removing waste products and extra fluid, and maintains balance of electrolytes such as sodium, potassium, chloride and calcium.
A proper diet also helps reduce the waste products that build up in the blood.One of the complications of long term diabetes is the end stage renal disease. Pancreatic diabetes mellitus (PDM) is a metabolic form of diabetes in which the pancreas is extensively damaged. One to eight percent of diabetic patients with end-stage renal disease (ESRD) suffer from diabetic nephropathy (dNP) due to pancreatic diabetes.
However, not much information is available that deals with pancreatic diabetes and ESRD. So, Gert Bodlaj and Georg Biesenback from the Department of Medicine, General Hospital Linz, Austria, conducted a study to investigate differences in the clinical outcome of the ERSD patients due to pancreatic diabetes or type2 diabetes. Type 2 diabetes usually results due to a resistance of the body cells to the action of insulin.
The researchers evaluated 96 diabetic patients who started hemodialysis in their dialysis center, of which 12 were diagnosed with pancreatic diabetes and the rest 84 patients were diagnosed with type2 diabetes.
Comparative studies were done on vascular risk factors and prevalence of vascular disease in both groups at the start of hemodialysis. Incidence of malnutrition and 5-year survival rates was evaluated in both groups.
The observation period of the study was five years.
• The vascular risk factors were similar in both groups.
• The HbA1c values were not different, however, the patients with PDM required significantly less insulin.
• The prevalence of vascular diseases at the start of dialysis was not significantly different between the two groups.
• The nutritional status at the start of hemodialysis was poor in the PDM patients. The frequency of underweight (BMI less than 21) was 50 percent in those patients versus 9 percent in those with type 2 diabetes.
• Death due to cardiovascular disease was 60 percent in the PDM group and 65 percent in the type 2 group. Infection was cause of death in 27 percent of the PDM patients and 21 percent of the patients with type 2 diabetes.
The study has limitations because of the small number of PDM patients (12 compared to 84 with type 2 diabetes), the absence of data on residual renal function, and the absence of more accurate methods of nutritional assessment.
The authors concluded – ‘The prevalence of vascular diseases is not significantly different in both, patients on hemodialysis with PDM versus type 2 diabetes. The lower survival of PDM patients can be related to poor nutrition status’.
Reference: Biesenbach G, Bodlaj G. Higher mortality of patients on haemodialysis with pancreatic diabetes compared to type 2-diabetes. Diabetol Metab Syndr. 2012 Mar 23;4(1):9. http://www.dmsjournal.com/content/pdf/1758-5996-4-9.pdf
Source-Medindia