Oral antibacterial agents may be effective alternatives to parenteral therapy for the treatment of chronic osteomyelitis.
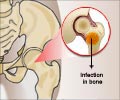
Osteomyelitis is an infection of the bone, most often caused by bacteria such as Staphylococcus aureus, although other microbes, including mycobacteria and fungi, are sometimes responsible.Osteomyelitis can be classified as acute or chronic. Unlike the acute form, which results from spread of bacteria through the blood, chronic osteomyelitis develops from fractures, open wounds, soft-tissue infections, and orthopedic implants.
Individuals with certain conditions or diseases that weaken the immune system such as diabetes, HIV/AIDS, sickle cell anemia and alcoholism are more prone to osteomyelitis.
Symptoms of osteomyelitis include redness, warmth, malaise, swelling and pain in the affected area, high fever, nausea and bone necrosis. Chronic osteomyelitis is diagnosed based on laboratory tests like erythrocyte sedimentation rate and C-reactive protein, imaging studies like x-ray and MRI, and microbiological examination that includes antibiotic sensitivity of infected tissues.
Current treatment consists of surgery plus a prolonged antibiotic therapy of 4 to 6 weeks. Surgery is necessary to remove the infected and devitalized bone and tissues. Up until fairly recently, administering oral antibiotics during this time period was rarely considered as a viable option. Oral therapy is now growing in popularity as evidenced by the fact that there are numerous studies conducted with oral agents. These studies have shown that oral antibiotics work equally well as parenteral agents to achieve adequate levels in bone.
Several oral antimicrobial agents have undergone evaluation for the treatment of acute and chronic osteomyelitis. They include fluoroquinolones such as ciprofloxacin, ofloxacin, levofloxacin, moxifloxacin; rifampin; linezolid; sulfamethoxazole-trimethoprim (SMX-TMP); aminopenicillins such as ampicillin and amoxicillin; and beta-lactamase inhibitors such as sulbactam and clavulanic acid.
In another study in osteomyelitis, the administration of parenteral ciprofloxacin followed by oral therapy was compared with IV ceftazidime. Two of three patients were cured with ciprofloxacin therapy, as were all three patients receiving ceftazidime.
In yet another study, Group A patients received IV cloxacillin followed by oral cloxacillin. Group B patients received a rifampin-cotrimoxazole combination. The overall cure rate in both groups after 10 years was nearly 90%, suggesting that oral SMX-TMP was an effective treatment option for chronic osteomyelitis.
All these studies indicate that oral therapy has been found to be nearly equivalent to parenteral therapy in chronic osteomyelitis. Oral and parenteral therapies have been shown to achieve similar cure rates; however, the advantages of oral therapy are that it avoids risks associated with intravenous catheters, provides excellent bone concentration and activity against targeted organisms, has reduced incidence of resistance, has fewer adverse effects even at high doses and is generally less expensive, making it a reasonable choice for treatment of osteomyelitis caused by susceptible organisms.
Reference: Oral Treatment Options for Chronic Osteomyelitis; Seher Khan et al; US Pharm. 2012;37(11):HS-2-HS-8.
Source-Medindia