Highlights
- Women who had their menses for the first time at the age of 13 or younger, are about 1.8 times more likely to suffer a stroke.
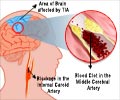
- The risk for cerebral infarction, in which //a section of brain tissue dies due to reduced blood flow and oxygen is also high.
- Women who stopped menstruating at 45 or younger are also more likely to get cerebral infarction, but not stroke.
Women who started their periods at the age of 13 or younger, are about 1.8 times more likely to suffer a stroke, than those who started at the age of 15. These women are also more at risk for cerebral infarction, in which a section of brain tissue dies due to reduced blood flow and oxygen.
Women who stopped menstruating at 45 or younger are also more likely to get cerebral infarction, but not stroke, compared to women who began menopause at the age of 50.
To study the relationship between stroke and menstruation, a research team led by Tohoku University and Teikyo University School of Medicine followed a group of 1,412 postmenopausal women in the rural town of Ohasama, Japan, between 1998 and 2010.
Through initial questionnaires and follow-up surveys, they tracked the women's ages of menarche and menopause, if and when they had a stroke, and other factors such as height, weight, heart disease and hypertension.
Studies by other groups found no strong association, but the researchers point out that most of those studies focused on the relationship between menarche and stroke mortality, not just stroke risk.
Menstruation onset is influenced by genetic, behavioral and socioeconomic factors, among others. Trying to delay menarche to help prevent stroke is a particularly interesting concept given that girls in developed nations are starting their periods earlier.
However, since the study only applied to a specific rural population, further research is required to conclude that delaying menarche would be an effective stroke prevention measure.
Reference
- Murakami K et al., Menstrual Factors and Stroke Incidence in Japanese Postmenopausal Women: The Ohasama Study, Neuroepidemiology (2016), DOI:10.1159/000452220.
Source-Medindia