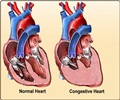
James A. Blumenthal, Ph.D., of Duke University Medical Center, Durham, N.C., and colleagues conducted a study to assess the effects of exercise on depressive symptoms and to determine whether reduced depressive symptoms were associated with improved clinical outcomes. The randomized controlled trial involved 2,322 stable patients treated for heart failure at 82 medical clinical centers in the United States, Canada, and France. A measure of depressive symptoms was gauged via a questionnaire (Beck Depression Inventory II [(BDI-II]). Depressive scores ranged from 0 to 59; scores of 14 or higher are considered clinically significant. Participants were randomized between April 2003 and February 2007 to receive either supervised aerobic exercise (goal of 90 min/week for months 1-3 followed by home exercise with a goal of ≥ 120 min/week for months 4-12) or to education and usual guideline-based heart failure care.
The median (midpoint) BDI-II score at study entry was 8; 28 percent of the sample had BDI-II scores of 14 or higher. Depression scores were available for 2,322 participants at the beginning of the study, 2,019 at month 3 and 1,738 at month 12. The researchers found that the adjusted 3-month BDI-II average score was 8.95 for the aerobic exercise group and 9.70 for usual care (a difference of -0.76). The adjusted BDI-II score at month 12 was 8.86 for the aerobic exercise group and 9.54 for usual care (a difference of -0.68).
The authors observed similar results when they examined the treatment effects within the subset of patients with clinically significant depressive symptoms (baseline BDI-II scores >14), with BDI-II scores at 3 and 12 months lower for patients in the aerobic exercise group than for patients in usual care group.
Patients within the aerobic exercise group who reported greater adherence to the exercise prescription achieved relatively larger reductions in depressive symptoms, although the absolute reduction was small.
The researchers also observed that elevated depressive symptoms were associated with more than a 20 percent increase in risk for all-cause mortality and hospitalizations and that the increased risk was independent of antidepressant use and established risk factors in patients with heart failure including age and disease severity.
Advertisement
Source-Eurekalert