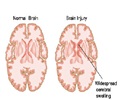
In early experiments with the tissue, researchers used it to examine chemical and electrical changes that occur immediately after brain injury and the changes that occur in response to a drug.
"This work is an exceptional feat. It combines a deep understand of brain physiology with a large and growing suite of bioengineering tools to create an environment that is both necessary and sufficient to mimic brain function,” said Rosemarie Hunziker, program director of Tissue Engineering at The National Institute of Biomedical Imaging and Bioengineering (NIBIB) in the United States.
According to project leader David Kaplan, a professor of engineering at Tufts and director of the Tissue Engineering Resource Center, this tissue offers advantages over using live animals to study brain injury.
In live animals, researchers are not able to start assessing the effects of a brain injury immediately after it occurs. That's because the animal's brain has to be dissected and prepared for experiments.
“With the new 3-D brain-like tissue, you can essentially track the tissue response to traumatic brain injury in real time. Most importantly, you can also start to track repair and what happens over longer periods of time,” Kaplan said.
Advertisement
The fact that we can maintain this tissue for months in the lab means we can begin to look at neurological diseases in ways that you can't otherwise because you need long timeframes to study some of the key brain diseases, Kaplan added.
Advertisement
Source-Medindia