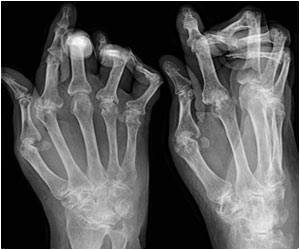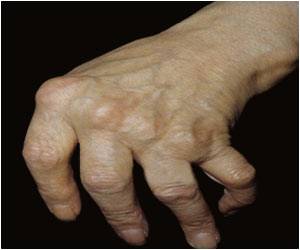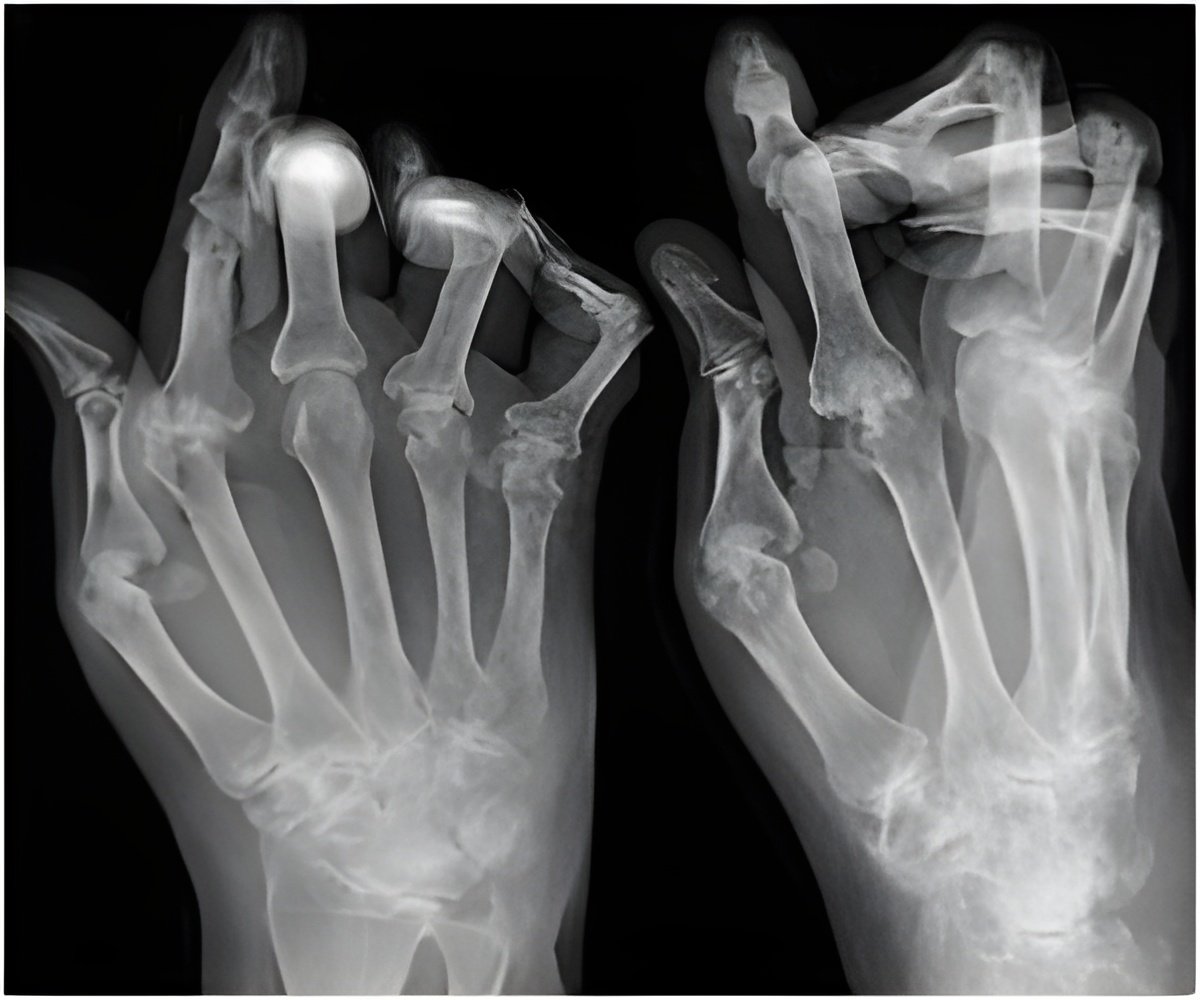
Medical conditions such as joint destruction and physical disability are outcomes of untreated rheumatoid arthritis. When prescribed alone to treat RA, traditional nonbiologic disease-modifying anti-rheumatic drugs (also called DMARDs) have proven to slow disease progression by nearly 20 percent. Anti-TNF therapies have been available in Ireland since 1999 and when combined with methotrexate for the appropriate patients, these drugs can eliminate all disease symptoms in up to 50 percent of patients with RA.
However, anti-TNF medications are expensive (the Irish average national cost in 2010 totaled $130 million) and the overall quality of life benefits when compared to total cost of using the drug, are often debated. To provide a better prospective about this debate, researchers from the St. Vincent''s University Hospital in Dublin, Ireland, evaluated the number of hospital inpatient days and musculoskeletal surgical procedures nationally in RA patients treated with anti-TNF therapy (the estimated total RA population in Ireland is 40,000).
"Maintaining a patients'' functional ability through appropriate use of anti-TNF drugs may ultimately provide health care savings that surpass the cost of the drugs whilst conferring greater health upon the patient," says Leonard C. Harty, co-investigator of the study from the department of rheumatology at St. Vincent''s University Hospital in Dublin, Ireland.
The researchers reviewed hospital occupancy records from 1995 to 2010 using the national database, the Hospital In-Patient Enquiry system. Data from 57 hospitals with patients admitted with a diagnosis of RA were included. Age group, number of inpatient days, gender and reason for admission were also recorded. National annual prescription data from 2000 to 2010 for anti-TNF usage was separately analyzed. Total numbers and averages were calculated as well as the average percent change. The association between anti-TNF usage, patient admissions to hospital and medical procedures was examined.
The research team reviewed 57,774 inpatient records of RA patients (of which 66 percent were female and the average age was 66 years-old). The analysis found that annual anti-TNF prescriptions increased 156 percent per year from 2,389 units in 2000 to 116,747 in 2010. The increase in anti-TNF prescriptions matched a decrease in RA inpatient days, resulting in a 13 percent reduction in hospital admissions. Significant cost savings were recorded as a result of fewer hospital days. Additionally, the study found an overall 47 percent reduction in total musculoskeletal surgical procedures from 2002 to 2010.This decrease in total musculoskeletal surgical procedures was significantly associated with increased usage of anti-TNF in people with RA.
Advertisement
The researchers note that additional factors other than anti-TNF therapy usage, such as improved use of non-biologic disease-modifying treatments and the prevention of other medical conditions, may have contributed to improved patient outcomes. Further analysis including the economic impact is currently underway.
Advertisement
Source-Newswise