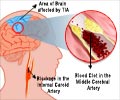
Blood thinner warfarin can increase risk of stroke in kidney disease patients on dialysis – quite opposite of the beneficial impact on individuals with abnormal heart rhythms.
People with atrial fibrillation, the most common type of abnormal heart rhythm, have a significantly increased risk of stroke. Blood thinners can mitigate this risk. However, almost no studies have examined whether warfarin can also prevent stroke in atrial fibrillation patients on dialysis.To investigate, Kevin Chan, Michael Lazarus, Raymond Hakim, (Fresenius Medical Care North America); and Ravi Thadhani, (Massachusetts General Hospital), studied 1,671 end stage renal disease (ESRD) patients with a diagnosis of atrial fibrillation who started dialysis in clinics operated by Fresenius Medical Care North America. Patients' health was monitored for an average of 1.6 years after dialysis was started.
The researchers found that patients who took warfarin increased their risk of stroke; however, the increase in risk was related to the degree of blood thinning in response to the drug. Dialysis patients whose blood was not monitored for warfarin levels after they received the drug had the highest risk of stroke (almost three-fold higher than patients not on warfarin). Notably, clopidogrel and aspirin—two other types of blood thinners—did not increase dialysis patients' risk of stroke.
Additional research is needed to determine why warfain has the opposite effect on stroke risk in kidney disease patients on dialysis compared with other individuals. One possible explanation maybe because bleeding is a well known complication of kidney failure and the concomitant use of blood thinners may exaggerate the risk of stroke from bleeding in the head. Also, this study's findings should be validated through randomized controlled clinical trials. "Until then, physicians should be cognizant of the possible risks associated with warfarin use for atrial fibrillation in ESRD patients with careful evaluation of the risks and benefits of intervention at the individual patient level," they concluded.
The study is appearing in an upcoming issue of the Journal of the American Society Nephrology (JASN).
Advertisement
GPL