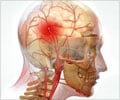
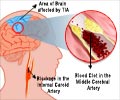
The focus on acute stroke in the UK government’s national stroke strategy may distract attention and resources from other important elements of stroke care, warn experts in a paper published on bmj.com today.
In 2005, the National Audit Office (NAO) report on stroke services outlined improvements for reducing death, disability and recurrent stroke, along with costs. Its recommendations led to the publication of the national stroke strategy in 2007.But it has been suggested that the NAO report overemphasised the benefits and cost savings to be gained from intravenous thrombolysis (giving anti-clotting drugs within three hours of an acute stroke) and underestimated the gains from comprehensive care in a stroke unit.
Now senior doctors at the University of Edinburgh warn that the report’s strong focus on hyperacute stroke care (the first 72 hours), and on greatly increasing the proportion of patients being given intravenous thrombolysis, could mean that the many other effective components of a comprehensive stroke service might not receive as much attention.
They examined the current performance of stroke services in England, Wales and Northern Ireland against three proven interventions for acute stroke: organised stroke unit care, early administration of aspirin, and intravenous thrombolysis.
According to the 2008 national sentinel stroke audit, 68% of patients admitted to hospital with an acute stroke spent more than half of their admission on a specialist stroke unit, 85% of eligible patients received early aspirin, and 1.4% of eligible patients received intravenous thrombolysis.
Based on these figures, the authors estimate that, at present, in a notional UK population of one million people, intravenous thrombolysis is preventing two patients from having a poor outcome (death or disability) each year, while stroke unit care and aspirin are preventing 37 and 24 poor outcomes respectively.
Advertisement
These calculations clearly show that the numbers of patients benefiting at current or realistic target levels are far larger for stroke units and aspirin than for intravenous thrombolysis, and they remain higher even at optimistic target levels, say the authors.
Advertisement
They conclude: “Although it is important to give intravenous thrombolysis in an appropriate setting to as many eligible patients as possible, it is crucial that this should not be at the expense of any of the other parts of a comprehensive stroke service. All elements of effective stroke care must be properly joined up, and funded, from hyperacute care to long term community support.”
Source-BMJ
SRM