"Our study reveals an important factor to explain why, as previous studies have shown, patients who have cardiac arrests in hospitals during daytime hours are more likely to survive," said senior author Benjamin Abella, an assistant professor of Emergency Medicine and clinical research director in Penn's Center for Resuscitation Science.
"These findings suggest that more attention to clinical emergency training and staffing at night may be an important way to improve hospital safety and patient outcomes."
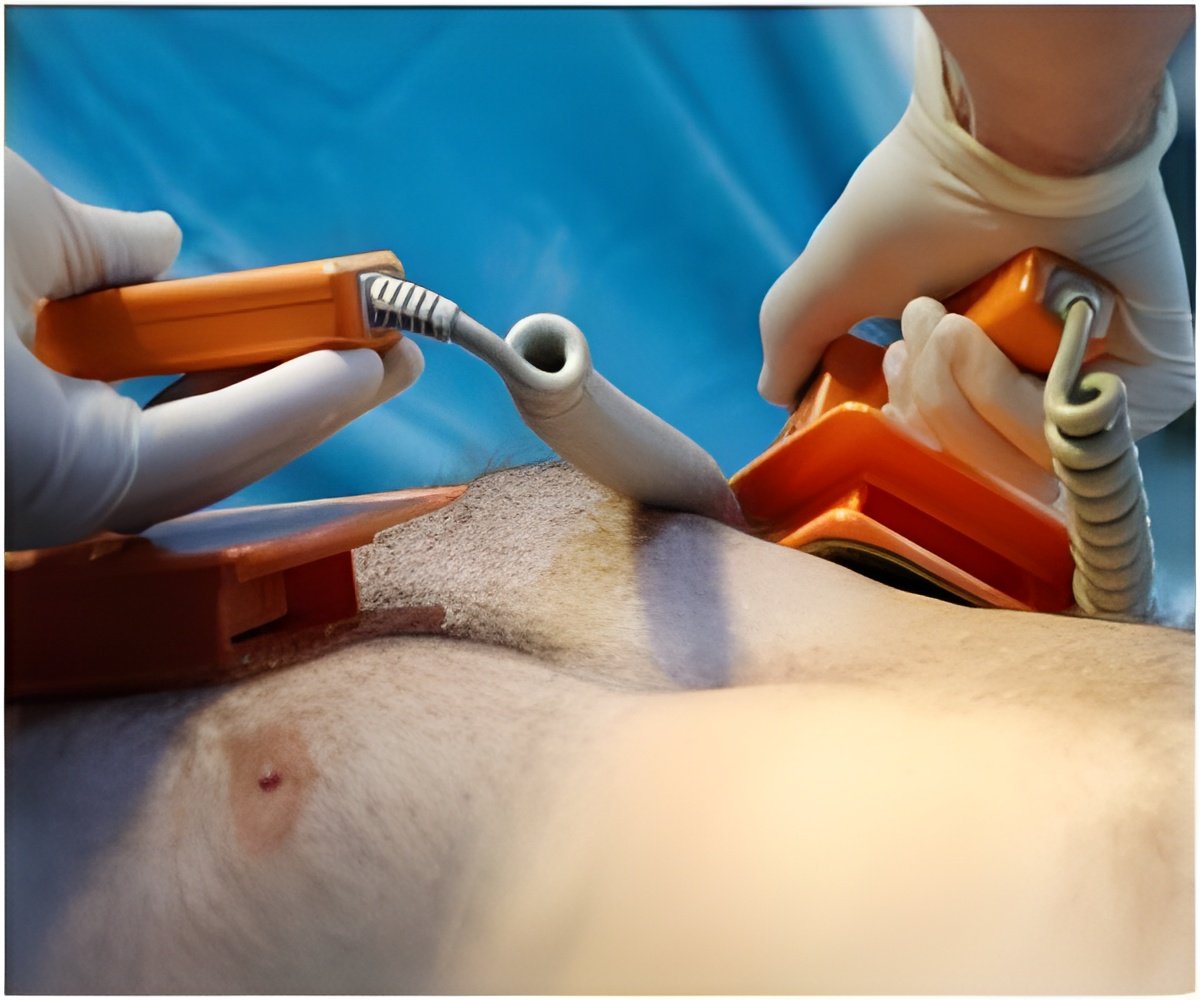
The authors studied 173 cardiac arrests that occurred in non-intensive care settings over the course of two years at three urban teaching hospitals.
The results showed that mean chest compression rate was lower during resuscitations that took place at night, between 11 p.m. and 7 a.m., compared to those during the day - 102 compressions per minute, with rates varying between 86 and 118, compared to 107, with variance between 100 and 114.
One hundred chest compressions per minute is the recommended rate, and previous research shows that when compressions are performed at lower rates, patients are more likely to die or suffer permanent brain damage from prolonged oxygen deprivation.
Advertisement
Among factors that the authors say may influence the variability in CPR quality between night and day: fatigue, lower staffing levels, and lack of supervision from supervising physicians, who are less likely to be present during overnight resuscitations.
Advertisement
Source-ANI