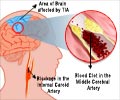
Despite advances in prevention, acute care, and rehabilitation, 20-30% of stroke patients in the UK die within a month and 13% of survivors are discharged to institutional care, according to experts in this week’s BMJ.
Their views follow a study published on bmj.com last month which found the more independent patients are six months after a stroke, the better their chances of long term survival.Despite undoubted progress, we still have much to do, argue Richard Thomson and Helen Rodgers from Newcastle University’s Medical Faculty.
For example, most acute trusts in the UK now have a stroke unit, but in 2006 only 62% of patients in the UK were admitted to a stroke unit and only 54% spent more than half of their inpatient stay on one, they say.
Thrombolysis (giving anti-clotting drugs within three hours of an acute stroke) reduces death and disability, yet in 2006 only 30 trusts in the UK provide this service, and even fewer provide it at all hours of the day, they add.
And, although up to 20% of stroke patients may be eligible for thrombolytic treatment, in 2006 only 218 patients – less than 0.5% of patients with acute ischaemic stroke in England, Wales, and Northern Ireland – received it.
Early supported discharge by a specialist stroke team can also improve outcome, yet provision of this service is limited.
Advertisement
Patients and their carers often report feeling abandoned after discharge and that they are badly informed and supported, both practically and emotionally.
Advertisement
Let us hope that these admirable aims will become the template for both commissioners and providers of care to seize the opportunity to enhance the health and wellbeing of a substantial and, to date, underserved group of patients, they conclude.
Source-BMJ
LIN/K