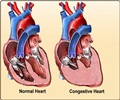
LVNC is an inherited heart muscle condition in which the muscular wall of the left ventricle appears to be spongy and non-compacted, consisting of a meshwork of numerous muscle bands (trabeculations). However, its cause, development, clinical course and treatment are the focus of ongoing research. As a result, the study authors said that the cardiology community's "understanding of the natural history of LVNC continues to evolve."
"Our ability to detect and recognize this condition has grown considerably over the past decade, as our imaging technologies have advanced," says study investigator William T. Katsiyiannis, MD, director of the Genetic Arrhythmia Center and a clinical cardiac electrophysiologist at the Minneapolis Heart Institute® at Abbott Northwestern Hospital in Minneapolis. "Fifteen years ago, the main tool to examine cardiac muscle was echocardiography, which was not as sensitive as it is today. Now, with the advent of cardiac MR [magnetic resonance], we are able to see far more detail of the heart."
While the current incidence rate of LVNC is unknown, Katsiyiannis hypothesizes that the condition may be far more common than has been previously postulated, due to a lack of diagnosis.
Previous data have indicated complications for patients with LVNC include stroke from blood clots that form in the non-compacted tissue, the development of heart failure or left ventricular dysfunction and the development of potentially dangerous ventricular arrhythmias.
To assess the association of LVNC with these traditional risk factors, the researchers assessed patients by echocardiography or cardiac MR, and diagnosed 125 patients with LVNC. Only 38.2 percent were diagnosed by echocardiography.
Advertisement
The study's patient population had a higher than expected incidence of congestive heart failure (38.5 percent), left ventricular dysfunction with ejection fraction of less than 45 percent by cardiac MR (31.9 percent) and ventricular tachycardia (24.8 percent). In addition, the researchers at Minneapolis Heart Institute® reported that 3.1 percent of patients experienced stroke and 3.1 percent experienced sudden death.
Advertisement
Source-Eurekalert