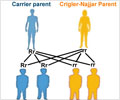
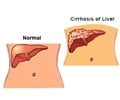
Results from their paired donor exchange programs for living donor liver transplantation (LDLT) have been released by two major transplant centers in Hong Kong and South Korea.
A single paired exchange, performed by the Hong Kong team under emergency circumstances, was a success. The Korean team reported 16 donor exchanges conducted over a 6-year period were successful. Full details of this novel approach to organ transplantation appear in the April issue of Liver Transplantation, a journal published by Wiley-Blackwell on behalf of the American Association for the Study of Liver Diseases (AASLD).Living donor transplantation has emerged as an alternative to the shortage of deceased donor organs, and in some parts of the world represents almost the only alternative for liver transplantation. However, many patients in need find that family members who are willing to donate organs have incompatible blood types. As a result, transplant centers worldwide are establishing coordinated donor exchange programs, where living donors are matched with medically acceptable and blood group compatible recipients in cases where the original intended recipient is not blood group compatible with their donor.
Paired donor exchange programs were adopted at two major transplant centers—The University of Hong Kong, Queen Mary Hospital, and the ASAN Medical Center, Seoul. Performing ABO-incompatible LDLTs, another practice that has emerged in response to the lack of blood-group compatible organs, generally requires a more stringent immunosuppressive regimen to allow the body to accept the organ. While this method has achieved some success, ABO-incompatible LDLT has a 5-year survival rate of only 52%. In addition, the heavier immunosuppressive regimen has uncertain long-term consequences and compromised quality of life.
Donor exchange programs appear to be an ideal solution to the shortage when only blood-group incompatible donors exist for a specific recipient. However, cultural obstacles to the idea exist. Lead researcher of the Korean team, Sung-Gyu Lee, M.D., explained, "The establishment of a paired exchange living-donor kidney transplantation program in Korea suggested that a similar program for LDLT would be acceptable in our country. In other Asian countries, such as Japan, where the availability of deceased donors is much less than in Korea, these programs may not be generally accepted." In Japan, the concept of giving or receiving organs to or from unrelated donors is not an accepted practice.
The donor exchange practice also raises ethical concerns, specifically, that all donors involved must understand the potential risks to their own health, as well as the possibility that while the recipient of their donated organ may survive, their own relative, for whose benefit they have entered into the exchange program, may experience an adverse outcome.
Chung Mau Lo, M.D., lead researcher of the Hong Kong team, commented, "Prior psychological evaluation and preparation in anticipation of possible scenarios are crucial in minimizing donor difficulties when confronting such mishaps. In fact, the donor should have a mindset that only with another compatible but unrelated donor donating, can the related recipient have an opportunity to undergo the LDLT." Furthermore, to ensure that all donors comply regardless of the surgical outcome, the LDLT operations must be conducted simultaneously, which may raise logistical issues.
Advertisement
Advertisement
RAS