Thyroid cancer that has spread to distant sites has a poor prognosis, but Amgen’s experimental drug inhibits tumor blood vessel formation and can slow disease progression in some patients, according to a researchers.
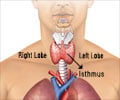
The investigational drug, motesanib diphosphate, is a VEGF inhibitor, a biologic agent that targets receptors on a protein known as vascular endothelial growth factor (VEGF). VEGF is instrumental in angiogenesis (formation of new blood vessels), a process that allows tumors to grow and spread.Study lead author Steven I. Sherman, M.D., chair and professor of M. D. Anderson's Department of Endocrine Neoplasia and Hormonal Disorders, noted strong evidence that VEGF receptors play an important role in metastatic thyroid cancer, a disease with few treatment options.
"There is no standard accepted chemotherapy for advanced metastatic differentiated thyroid cancer, and response rates have typically been 25 percent or less," Sherman said. "Most patients are not treated with systemic chemotherapy because the limited benefit rarely justifies the side effects. Treatment of thyroid cancer has been a completely unmet need."
Sherman, colleagues in 10 countries, and scientists from Amgen, which is developing motesanib diphosphate (AMG 706), planned and conducted one of the largest clinical trials ever done for metastatic thyroid cancer.
Of the 93 patients with rapidly progressing cancer who were enrolled in the study, 49 percent had a positive response. From that group 14 percent had their tumors shrink and 35 percent had their tumors stabilize for more than 24 weeks. Median progression-free survival was estimated to be 40 weeks.
Genetic analyses of 25 patients indicated that those with a specific mutation known as BRAF V600E in their tumors had a better response to motesanib diphosphate than did those without the mutation. Additional research is needed on this genetic connection, but the early results are a good start, Sherman said.
Only 15 percent survive for 10 years
But about 15 percent of patients will develop distant metastases, typically to the lungs. A small percentage of these patients will respond well to radioactive iodine treatment and survive for many years. But for others, the estimated median survival duration is two to four years, with a 10-year survival rate of less than 15 percent.
Multinational trial
Forty-two institutions internationally participated in the clinical trial, including an important collaboration with the Institut Gustave Roussy, M. D. Anderson's sister institution in Villejuif, France. The study enrolled patients with progressive, locally advanced or metastatic, radioiodine-resistant thyroid cancer.
Study participants took 125 milligrams of oral motesanib diphosphate once a day for 48 weeks or until they experienced unacceptable side effects or disease progression. The primary treatment outcome was radiographic evidence of tumor shrinkage as determined by an independent review. The researchers also analyzed the duration of tumor response, progression-free survival, and drug safety.
Stable Disease in 67 percent of patients
The researchers monitored tumor response with computed tomography (CT) or magnetic resonance imaging (MRI) scans of the neck, chest, and abdomen every eight weeks or in response to signs of disease progression. Partial or complete responses to the drug were evaluated by independent review and confirmed with repeat scans four or more weeks later.
Thirty-two patients completed the full 48 weeks of treatment. Motesanib diphosphate was discontinued in 35 patients because of disease progression and in 12 patients because of drug-related adverse events. Five patients died, and nine withdrew for various administrative or personal reasons.
Thirteen patients (14 percent) achieved an objective partial response to the drug. Sixty-two patients (67 percent) experienced stable disease during the study; 33 of these (35 percent) achieved durable stable disease for at least 24 weeks. Nine patients (10 percent) had unconfirmed partial responses, which were classified as stable disease. Seven patients (8 percent) experienced only disease progression, and no response information was available for 11 patients (12 percent) because of incomplete or uninterpretable radiographic scans.
Eighty-seven patients (94 percent) experienced at least one treatment-related adverse event. The most common events were diarrhea, hypertension, fatigue, and weight loss. In 51 patients, the adverse events were classified as severe (grade 3). Five patients had grade 4 (life-threatening) adverse events, including low calcium levels, high levels of uric acid, low potassium levels, cerebral hemorrhage, mental confusion, agitation, or decreased urine production. Two patients whose disease had progressed died of pulmonary hemorrhage.
Phase I Program Revealed Drug's Potential
The drug's potential benefit for advanced thyroid cancer was identified by researchers in M. D. Anderson's innovative Phase I Clinical Trials Program, led by Razelle Kurzrock, M.D., chair and professor of M. D. Anderson's Department of Investigational Cancer Therapeutics.
The program typically has about 80 Phase I clinical trials under way, testing new targeted therapies for the first time in cancer patients. In addition to closely monitoring a new drug for safety, the program tests it against many different types of cancer.
"The molecular targets of new potential drugs are important for cancer in general, but at this stage the drugs aren't specific for any one type of cancer, so we include patients with different types on these early studies," Kurzrock said. "This gives us a unique opportunity to see response signals for the first time in specific cancers, flagging a drug for more extensive study in phase II or phase III clinical trials."
Source-Newswise
SRM