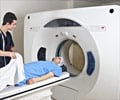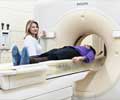
Use of medical imaging has grown rapidly in recent years, but along with the potential benefits has come an increase in the amount of ionizing radiation associated with many such tests and the accompanying potential risks of cancer. "Although much attention has been paid to radiation from computed tomography (CT) scans, a recent study demonstrated that the single test with the highest radiation burden, accounting for 22 percent of cumulative effective dose from medical sources, is myocardial perfusion imaging (MPI). Volume of MPI increased from less than 3 million procedures in the United States in 1990 to 9.3 million in 2002, and it is now estimated to account for more than 10 percent of the entire cumulative effective dose to the U.S. population from all sources, excluding radiotherapy," according to background information in the article. Few data are available to characterize the total radiation burden received over an extended period by patients undergoing MPI.
Andrew J. Einstein, M.D., Ph.D., of Columbia University Medical Center and New York-Presbyterian Hospital, New York, and colleagues analyzed procedures involving ionizing radiation received by a group of patients who received MPI to evaluate the total numbers of MPI examinations, other tests involving radiation, cumulative effective doses of radiation, and clinical indications for testing and repeat testing. The study included 1,097 patients undergoing MPI during the first 100 days of 2006 (January 1-April 10) at Columbia University Medical Center. The researchers evaluated all preceding medical imaging procedures involving ionizing radiation undergone beginning October 1988, and all subsequent procedures through June 2008, at the center.
Patients underwent a median (midpoint) of 15 procedures involving radiation exposure, of which 4 were high-dose procedures, defined as an effective dose of at least 3 mSv (millisievert; a measure of radiation dose), the equivalent of 1 year's natural background radiation. A total of 200 patients (18.2 percent) had at least 3 MPIs and 4.9 percent had at least 5 MPI examinations.
The researchers found that the median cumulative estimated effective dose from MPI alone was 28.9 mSv, and for all medical testing, was 64.0 mSv. A total of 71 patients (6.5 percent) received cumulative doses of more than 100 mSv due to MPI alone, and 31.4 percent of patients received more than 100 mSv from all medical sources, including 120 patients (10.9 percent) who received cumulative dose of more than 200 mSv.
The primary reason for testing was chest pain, breathing difficulty, or both in 66.8 percent of examinations. More than 80 percent of initial and 90 percent of repeat MPI examinations were performed in patients with known cardiac disease or symptoms consistent with it. Of 1,097 patients undergoing index MPI, 38.6 percent underwent additional MPI studies. For this group of patients undergoing multiple MPIs, the median cumulative estimated effective dose was 121 mSv.
Advertisement
"Our study reveals very high cumulative estimated effective doses to many patients undergoing MPI, and especially to patients undergoing repeat MPI testing. More than 30 percent of patients received a cumulative estimated effective dose of more than 100 mSv, a level at which there is little controversy over the potential for increased cancer risks," the authors write. "Efforts are needed to decrease this high cumulative dose and its potential attendant risks."
Advertisement
Source-Eurekalert