This is one of the first studies to examine how conformity with current and emerging heart-failure quality measures can impact patient survival and outcomes in the outpatient setting.
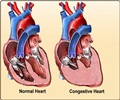
A chronic, progressive disease, heart failure impacts millions and results in morbidity, death, the use of significant health care resources, and significant costs. While quality-of-care measures based on national guidelines from the American College of Cardiology and the American Heart Association have been developed, and while prior studies have shown that performance-improvement initiatives substantially improve conformity with these measures, it was unclear if these efforts could improve survival in the real-world clinical practice setting.
"This study establishes a strong process-of-care–clinical outcome link and provides evidence that specific heart failure therapies effectively improve patient survival in an outpatient setting," said the study's first author, Dr. Gregg C. Fonarow, UCLA's Elliot Corday Professor of Cardiovascular Medicine and Science and director of the Ahmanson–UCLA Cardiomyopathy Center at the David Geffen School of Medicine at UCLA. "These results have significant clinical and public health implications in helping track and improve quality of care and heart-failure patient outcomes."
For the study, researchers examined data on 15,177 heart failure patients seen at 167 cardiology practice clinics in the U.S. The data was taken from a national quality improvement program called the Registry to Improve the Use of Evidence-Based Heart Failure Therapies in the Outpatient Setting (IMPROVE HF).
Researchers reviewed medical records at the beginning of the implementation of the IMPROVE program and followed up at 12 and 24 months to assess the relationship between adherence to seven nationally recommended treatment measures and patient outcomes.
Advertisement
- Three types of heart failure medications, including beta blockers, aldosterone antagonists, and angiotensin-converting enzyme inhibitors or angiotensin receptor blockers.
- The use of cardiac resynchronization therapy, a device that helps coordinate heart contractions.
- Anticoagulant therapy for atrial fibrillation, to prevent clot formation in patients with an irregular heart beat.
- The use of implantable cardioverter-defibrillator devices, to deliver electrical shocks if potentially fatal heart rhythm abnormalities occur.
- Heart-failure patient education.
Advertisement
Researchers found that six out of the seven individual measures were associated with significantly improved patient survival over 24 months. The odds of mortality reduction ranged from 31 percent for anticoagulant therapy to 55 percent for beta blocker use, compared with eligible patients who did not receive these therapies.
In a summary score reflecting adherence to the quality measures, each 10 percent increase in the composite score was associated with 13 percent lower odds of 24-month mortality.
Researchers also looked at an "all or nothing" score that found patients who received all the therapies for which they were eligible had 38 percent lower odds of mortality, compared with patients who did not receive one or more of the therapies for which they were qualified.
Previous research by this team showed how the use of IMPROVE HF, a performance-improvement intervention program, helped increase adherence to these national guideline–related therapies but didn't address the impact on patient outcomes.
The current study provides definitive evidence that complying with measures based on six out of seven of these national guideline therapies is linked to favorable clinical outcomes, with lower mortality over 2 years.
"Adhering to these critical, evidence-based, national guideline–recommended treatments for heart failure truly made an important difference in real-world heart-failure patient survival,"
Fonarow said. "This research puts quality-improvement interventions front and center as an effective means to improve outcomes for outpatients with heart failure."
Fonarow added that the next step is to implement performance-improvement intervention programs in every outpatient practice in which heart failure patients are cared for to further enhance adherence to these recommended therapies and to improve clinical outcomes.
Currently, two guideline-recommended therapies, implantable cardioverter-defibrillator devices and cardiac resynchronization therapy, are not included as national heart-failure performance measures. According to Fonarow, the link to improved survival demonstrated with these two measures suggests these are valid and useful measures of heart failure quality.
The only measure that was not associated with improved 24-month survival was use of aldosterone antagonists. More study will need to address whether this is a useful heart-failure quality measure.
Medtronic Inc., a manufacturer of cardiac resynchronization therapy and implantable defibrillator devices, provided financial and material support for the IMPROVE HF registry. The company had no role or input in the selection of end-points or quality measures used in the study.
Fonarow has received honoraria and consultant fees from Medtronic. Additional author financial disclosures are listed in the study manuscript.
Source-Eurekalert