Two studies that may influence clinical treatment of serious eye conditions appear in the July issue of Ophthalmology, the journal of the American Academy of Ophthalmology.
One study reports on silent cerebral infarcts (SCI) incidence and visual field loss in patients with normal-tension glaucoma; the other correlates inflammation biomarkers with corneal transplant rejection in herpes simplex patients.Silent Cerebral Infarcts: Risk Factor for Visual Field Loss as Well as for Stroke?
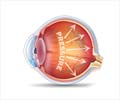
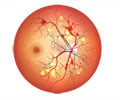
Health conditions in normal tension glaucoma (NTG) patients differ from those in patients with the more common primary open-angle glaucoma (POAG). For one thing, an increased incidence of silent cerebral infarct (SCI), blockage in small blood vessels in the brain, is seen in brain scans of people with NTG. Also, visual field loss is often more rapid in NTG patients than in those with POAG. Researchers at The Chinese University of Hong Kong, led by Dexter Y.L. Leung, FRCS, recently investigated whether SCI might be directly related to rate of visual field loss in patients newly diagnosed with NTG.
They found that visual field loss was 61 percent more likely in NTG patients with SCI than in those without SCI. Computed tomography (CT) brain scans performed at the beginning of the study showed that of 286 study subjects with similar NTG disease factors, 64 had SCI and 222 did not. Patients' visual field status was assessed every four months over three years. Though this study was in newly diagnosed NTG patients and results could vary in patients who have been in treatment, the results raise important points.
"First, this study adds weight to the hypothesis that vascular factors are likely causes of NTG, along with intraocular pressure (IOP). Second, if additional studies confirm SCI as a risk factor for visual field loss, treatment to prevent SCI might slow disease progression in NTG patients. Third, brain scans of NTG patients to detect SCI might be deemed cost-effective. Since treating SCI is also known to prevent stroke, we may be talking about saving not only vision, but lives," said Dr. Leung.
NTG is termed "normal" because the IOP, the pressure within the eye, is lower than the point at which optic nerve damage is known to occur in POAG patients. Despite this "normal" IOP, optic nerve damage does occur in NTG patients, who comprise about one-third of all people with glaucoma.
Advertisement
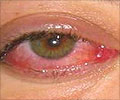
The herpes simplex virus (HSV) can infect the eye and sometimes causes so much damage that the person's cornea must be replaced with a transplant. (The cornea is the clear covering of the front of the eye that helps focus light for vision.) Doctors knew transplants were more likely to fail in people with HSV than in patients with other disorders, such as keratoconus, an abnormal steepening of the cornea. This higher failure rate occurred even when HSV infection did not appear to be active in patients. Researchers at the Kellogg Eye Center, University of Michigan, theorized that such patients might have corneal inflammation that could not be detected upon clinical examination but might increase the risk of transplant rejection.
Advertisement
"It is also possible that treating inflammation intensively before corneal transplant surgery would reduce the risk of rejection," said Dr. Roni M. Shtein, MD, MS, cornea specialist and lead author of the report.
Source-Eurekalert
RAS