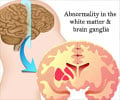
Doctors at the University of Minnesota Children’s Hospital, Fairview have performed the first ever bone marrow and cord blood transplant on an 18-month-old boy to treat recessive dystrophic epidermolysis bullosa (RDEB).
The boy, who has received both umbilical cord blood and bone marrow from a perfectly matched sibling, has the most severe form of RDEB, which also causes skin to slough off on the inside of the body, affecting the mouth, esophagus, and gastrointestinal tract.The doctors have already used bone marrow to successfully cure the disease in mice, along with collaborators from Columbia University.
They tested various types of adult stem cells to determine which would give rise to the development of type VII collagen, the protein that people with RDEB lack. One type of immature cells from bone marrow proved to be the best at producing anchoring fibrils that bind the skin to the body.
'Our goal is to determine the usefulness of stem cells, whether from the umbilical cord blood or adult tissues like bone marrow, in the treatment of human disease,' said Dr. John E. Wagner, professor of Pediatrics and director of the Division of Hematology, Oncology, and Blood and Marrow Transplantation and director of clinical research of the Stem Cell Institute at the University of Minnesota.
'There are hundreds of thousands of children and adults waiting for new breakthroughs in stem cell research, and time is never enough. In two years, the team was able to move this project forward remarkably fast—from testing in animal models to treating patients. Time will tell whether this risky treatment will work as effectively in humans. But, RDEB is a horribly debilitating, life-threatening disease with no existing curative therapy,' he added.
The doctors anticipate in early 2008, approximately 100 days after transplant, they will be able to judge whether this the treatment helped.
Advertisement
'This represents a real change in thinking within the dermatological community. The possibility of this approach compels us to explore more broadly the way some skin diseases are typically treated,' said Dr. Maria Hordinsky, head of the Department of Dermatology at the University of Minnesota and member of the care team.
Advertisement
SRM/B