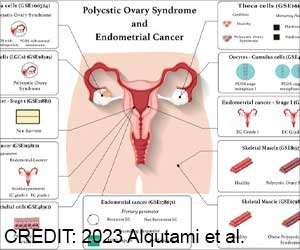
Europeans tend to overestimate benefits of breast and prostate cancer screening, researchers say.
In Wednesday's online issue of the Journal of the National Cancer Institute, Gerd Gigerenzer, of the Max Planck Institute for Human Development in Berlin, and colleagues said 92 per cent of women surveyed believed the life-expectancy benefit from mammography screening is at least 10 times higher than it really is, or said they did not know how much it helped.Among men, 89 per cent overestimated the benefit of prostate-specific antigen or PSA screening by a factor of 10 or more, or said they did not know about the level of benefit.
"Knowing the benefit of a treatment is a necessary condition for informed consent and rational decision making," the study's authors wrote, based on their review of pamphlets given out by government-run mammography screening programs in seven European countries.
The researchers also surveyed more than 10,200 people from Austria, France, Germany, Italy, the Netherlands, Poland, Russia, Spain and the United Kingdom to assess perception of the risks and benefits of the two screening programs.
"In the countries investigated, physicians and other information sources appear to have little impact on improving citizens' perceptions of these benefits," the study's authors concluded.
In an editorial accompanying the study, Dr. Lisa Schwartz and Dr. Steven Woloshin of the Dartmouth Institute for Health Policy & Clinical Practice in Hanover, said accurate screening messages should be more prominent in pamphlets from government-run mammography screening programs.
Advertisement
The database for prostate cancer screening is much smaller, with results from two randomized trials coming to different conclusions. A summary in the editorial showed an estimated 0.7 fewer deaths for every 1,000 men aged 55 to 69 who are screened over nine years, and the other found no lower risk of dying with prostate cancer screening also over nine years.
Advertisement
"Most importantly, screening leads to overdiagnosis of some cancers never destined to cause harm," they wrote. "People who are overdiagnosed cannot experience any benefit from screening — they can only experience the anxiety of unnecessary diagnosis and the harms of unnecessary treatment."
They also said the researchers' methods were biased toward overestimation based on the design of the survey, and that it's not clear if the study participants were truly representative of the European Union.
"We need to move from selling screening to helping people realize that screening is a genuine choice," Schwartz and Woloshin said. "That means routinely giving people the information needed to make these choices."
Source-Medindia
GPL





![Prostate Specific Antigen [PSA] Prostate Specific Antigen [PSA]](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)