A 2009 review by the Academy of the safety and efficacy of a widely used corneal transplant procedure and a warning about an unusual but serious reaction to systemic fluroquinolones, are the highlights of September’s Ophthalmology, the journal of the American Academy of Ophthalmology (Academy).
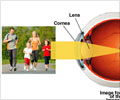
DSEK Deemed Safe, Effective Treatment for Corneal DiseasesDescemet’s Stripping Endothelial Keratoplasty (DSEK) corneal transplant procedure is a safe and effective treatment for corneal endothelial diseases, says a 2009 review by the cornea panel of the Academy’s Ophthalmic Technology Assessment Committee, led by W. Barry Lee, M.D. The panel reached this conclusion through a comprehensive review of pertinent studies published from 1980 to 2009. Eighty-five percent of corneal transplants performed in the United States are associated with endothelial diseases. The cornea is the eye’s clear outer tissue that refracts, or bends, incoming light to focus images on the retina at the back of the eye; the endothelial layer lines the back surface of the cornea and regulates water levels (hydration). In February 2009 the Board of Trustees approved the corneal panel’s conclusions for use in official Academy statements.
In outcome comparisons derived from the review, DSEK was superior to penetrating keratoplasty (PK)–the dominant procedure prior to DSEK’s development–in terms of earlier recovery and stability of vision, refractive status after surgery, and specific risks and complications associated with surgery and recovery. The most common DSEK complications apparently do not hinder ultimate recovery of vision in most patients. DSEK and PK outcomes were similar in terms of survival of the transplanted cornea, visual sharpness (acuity) and endothelial cell loss, and specific surgical risks and complication rates.
"To further improve DSEK and related procedures and provide the best patient care, we need prospective clinical studies to set expectations for long-term endothelial cell survival and to determine acceptable complication rates," Dr. Lee said. "Another important research area is how to improve tissue (donor cornea) preparation and surgical techniques to increase endothelial cell survival," he added.
Seeing Double? A Type of Antibiotic May be the Cause
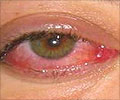
A 2009 study finds that a class of antibiotics known as fluoroquinolones, administered systemically to treat a broad range of bacterial infections, may cause double vision (diplopia) in some patients. Researchers at the Casey Eye Institute, Oregon Health Sciences University (OHSU), launched the first investigation of this problem after the National Registry of Drug-Induced Ocular Side Effects at OHSU received multiple reports of diplopia associated with systemic fluoroquinolones. This antibiotic type has side effects not seen with other antibiotics, including tendon dysfunction, and it is possible that tendinitis in the muscles around the eyes could cause double vision. Fluoroquinolones treat infections including bacterial or chronic bronchitis, pneumonia, sinusitis, and some skin infections.
Advertisement
"Doctors need to be aware of this potential reaction when prescribing these antibiotics and consider stopping therapy if diplopia occurs," Dr. Fraunfelder said. He also said that special care should be taken with patients who are older than 60, have had renal failure, or are taking steroids, and that thorough ophthalmic and neurological exams should be done to rule out other causes of double vision.
Advertisement
Source-Eurekalert
RAS