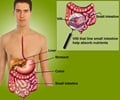
Celiac disease is a digestive disorder triggered by the protein gluten.
"We found that having elevated levels of IL-15 in the gut could initiate all the early stages of celiac disease in those who were genetically susceptible, and that blocking IL-15 could prevent the disease in our mouse model," said Bana Jabri, associate professor of medicine and pathology of the University.
"It also demonstrated that in the treatment of inflammatory intestinal diseases, vitamin A and its retinoic acid metabolites are likely to do more harm than good," she said.
"In a stressed intestinal environment retinoic acid, which was thought to lessen inflammation in the intestine, acted as an adjuvant that promoted rather than prevented inflammatory cellular and humoral responses to fed antigen," the authors note.
Gluten can trigger an autoimmune reaction in the intestines of genetically susceptible people. This prevents the proper absorption of food and nutrients, and causes a variety of gastrointestinal and extra-intestinal symptoms.
Advertisement
They knew that many patients with this disease had high levels of Interleukin 15 in their intestines.
Advertisement
When they blocked IL-15, however, the diseased mice reverted to normal, and were once again able to tolerate gluten.
The study appeared in the journal Nature.
Source-ANI